Custom Telehealth Software for Stroke Care
Features, Costs, and Benefits
In healthcare IT since 2005, ScienceSoft designs and develops advanced telemedicine software for stroke care management.
The Essence of Telestroke
Telestroke connects experienced vascular neurologists with several emergency care hospitals to provide online consultations on efficient stroke treatment using telehealth technology and remote patient monitoring. According to Harvard Medical School, telestroke helps lower mortality risks and improve care outcomes.
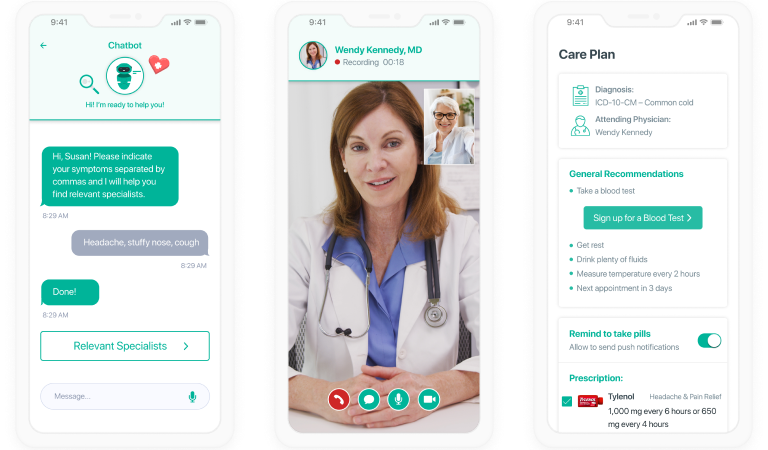
Custom telestroke software offers tailored functionalities and workflows to initiate real-time remote assessment, diagnosis, and treatment planning. It helps healthcare providers to react swiftly in critical moments and integrates tools for emergency care coordination and post-stroke rehabilitation management.
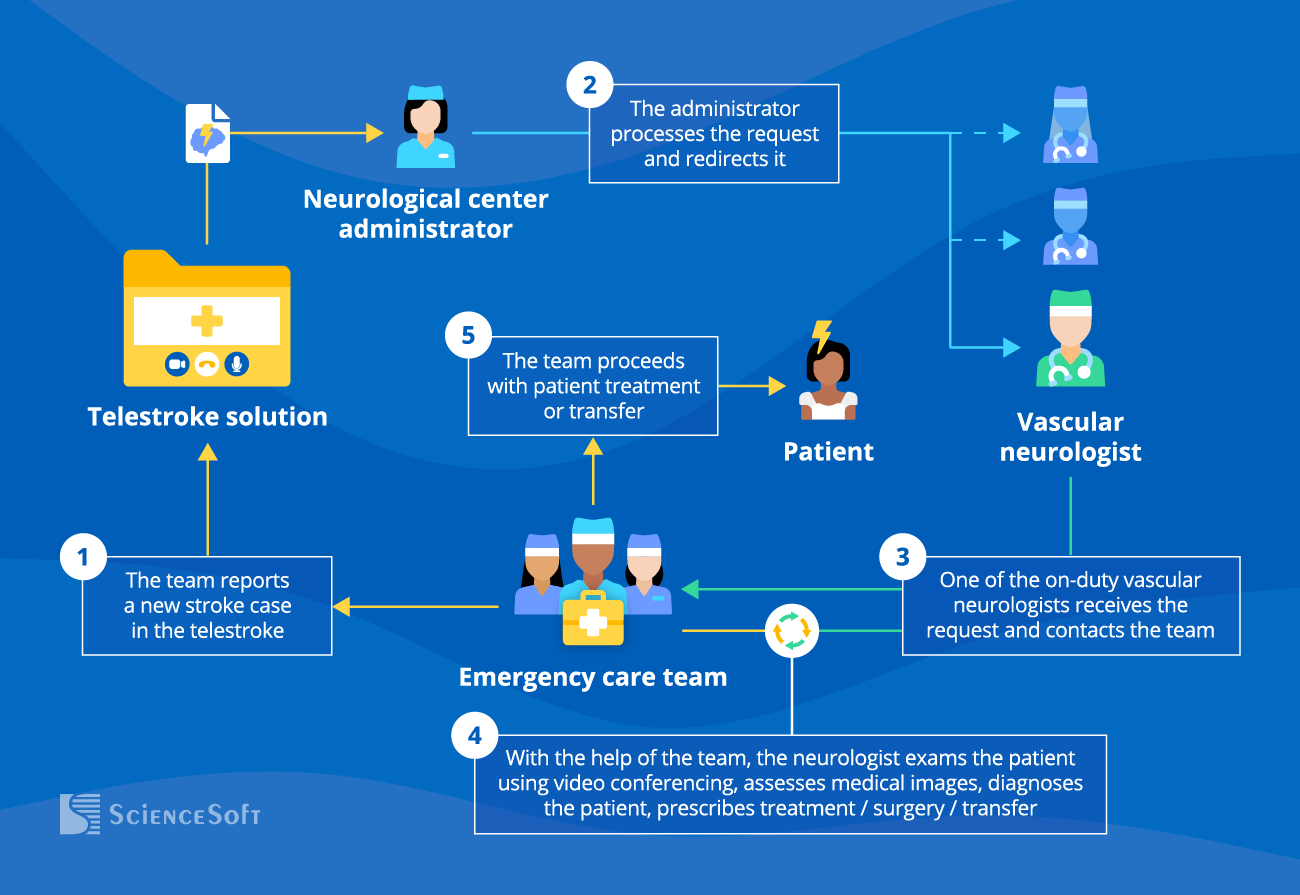
With a telestroke solution, patient care is delivered as follows:
Telemedicine is effectively used to diagnose and help treat all major stroke types:
- Ischemic stroke – brain dysfunction caused by lack of blood flow (ischemia).
- Hemorrhagic stroke – bleeding into the brain or between the brain's membranes caused by the rupture of a blood vessel.
- Mini-stroke or transient ischemic attack – a brief episode of ischemia with symptoms lasting less than 1-2 hours.
The Architecture and Integrations of Telestroke Software
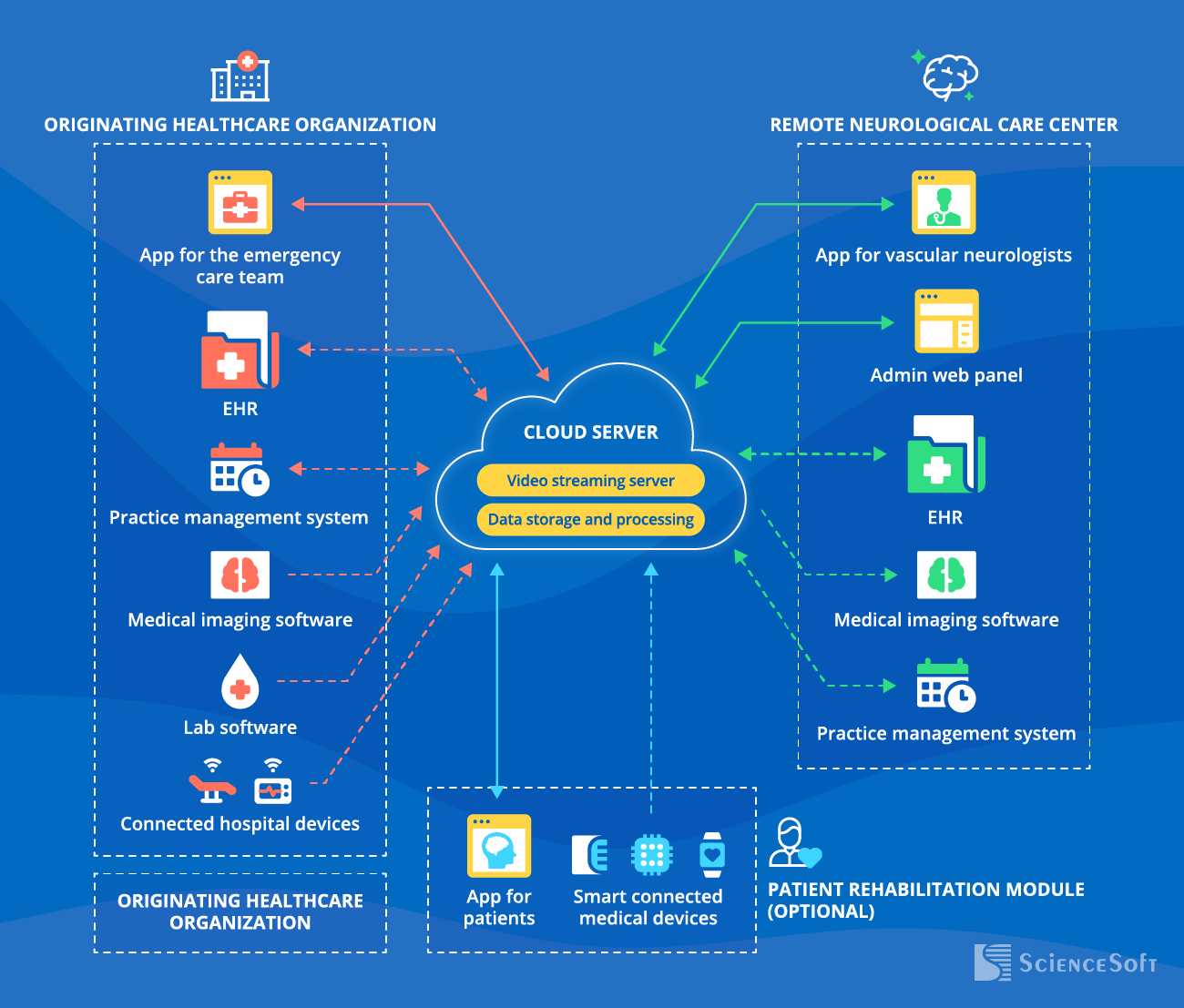
The core part of a telestroke solution is a cloud server with a data storage and processing module and a video streaming server. The former enables secure storage and handling of medical data and ePHI (e.g., device-generated data, treatment plans). The latter provides real-time audiovisual communication between an emergency care team, a vascular neurologist, and a patient. The user-facing modules of a telestroke solution usually include the following:
App for the emergency care team
to launch a real-time or follow-up stroke consultation with a vascular neurologist, view a patient’s treatment plan, etc.
App for vascular neurologists
to examine a patient, assess the stroke symptoms, and provide online consultations.
Admin web panel (for admins, health services managers)
to manage software access rights, assign consultation requests, and monitor the quality of services (audio/video quality, consultation timings, etc.).
A patient rehabilitation module (optional):
App for patients
to schedule and join follow-up appointments and rehabilitation sessions, log symptoms, and check in-app treatment plans. Depending on a patient’s condition, the app can be operated by a relative or caregiver.
Smart medical devices
to ensure automation in measuring and collecting the patient’s vitals for further analysis. Recommended devices: blood pressure monitor, ECG patch, smartwatch.
Important integrations to ensure fast and secure access to patient health data:
to provide access to medical history, chronic conditions, and allergies for a vascular neurologist. The patient’s medical and contact information from the originating site’s EHR should be automatically uploaded to the neurological center’s EHR for treatment, billing, etc.
Medical imaging and laboratory software
to get an instant view of diagnostic images and lab test results, identify the stroke type, the vessel blockage location, and decide on the treatment. Medical images (e.g., CT scans, MRI scans) can be transferred via API to the cloud server for image analysis or analyzed by the vascular neurologist via a DICOM viewer.
to access the healthcare specialists’ schedules (of the neurological center and the originating site), automate billing, etc.
Connected hospital devices or sensors
to provide a vascular neurologist and a care team with real-time patient vitals for streamlined diagnosing and symptoms monitoring.
Which hospital gets reimbursement for telestroke services?
CMS-regulated payers (e.g., Medicare, Medicaid) reimburse the services of the originating site and the neurological center. To receive reimbursement, both organizations should log the stroke case in their EHRs with the billing codes according to CMS guidelines.
Key Features of Telestroke Software
When designing a unique feature set for a telestroke solution, ScienceSoft's healthcare IT consultants consider each client's unique business needs and requirements. Here is the list of common features we implement:
How to Build Telestroke Software
ScienceSoft always follows a meticulously planned development roadmap to ensure custom telestroke software is reliable, secure, and compliant with the stringent industry requirements.
1
Analyzing requirements and introducing the feature set
Understanding the specific needs of stroke care providers and patients to identify essential features, such as remote patient monitoring, brain scan analysis tools, automated triage algorithms, and stroke severity scoring.
2
Defining the architecture and tech stack
Designing a scalable and secure software architecture; selecting technologies and frameworks aligning with industry standards and prioritizing low-latency communication for real-time doctor-patient interactions.
3
Project planning
Defining the budget, timeline, deliverables, KPIs, and resource allocation.
4
Iterative development and testing
Creating prototypes, validating the idea with the stakeholders (stroke care experts, neurologists, emergency physicians, and radiologists), carrying out agile development and testing in parallel.
5
Deployment
Setting up servers, implementing rigorous security measures to protect patient data, and ensuring seamless integration with existing healthcare systems (e.g., EHR/EMR, hospital information systems) and smart devices (e.g., a hemiplegia finger training device, a wearable carotid Doppler device, a PPG device).
6
Maintenance
Providing continuous support and upgrades based on user feedback and emerging needs in stroke care; ensuring ongoing regulatory compliance.
How Much Does Telehealth Software for Stroke Care Cost?

A telemedicine solution for stroke care with core features like online consultations, chat, file exchange, and EHR integration usually costs from $150,000 to $200,000. The costs may increase to $300,000 for an advanced solution with features like integrated devices, medical image analysis, AI, etc.
Want to understand the detailed costs of your telestroke software?
Learn more about telemedicine software development cost factors and ROI.
Benefits of Telestroke Solutions
For neurological centers
Service coverage expansion and increased capacity of treated patients (Healthcare IT News).
General benefits
- Reduced time from patient admission to stroke treatment (door-to-needle time) due to quick access to neurological care (National Library of Medicine).
- Decreased risk of stroke-related complications and disabilities due to timely treatment decisions (The Harvard Gazette).
- Minimized patient transfers leading to lower expenses and risks (for patients who need non-surgical treatment) due to faster care delivery backed up with expert consulting at the local ER (American Academy of Neurology).
- Improved diagnostic accuracy in emergency care due to close collaboration with vascular neurologists (Journal of Clinical Medicine).
What Determines Telestroke Software Success
Telestroke software success highly depends on its ability to provide timely care. ScienceSoft's consultants defined factors helping to ensure it with technology:
|
|
Clear UXto make user journeys simple and save the time of the medical staff involved in stroke care. |
|
|
Seamless integration with required systemsto provide a vascular neurologist with an integrated patient view, timely access to all needed patient information via EHR, LIS, medical imaging software, etc., resulting in quality stroke care. To keep all data easily accessible, ScienceSoft suggests using widely adopted standardized APIs (e.g., FHIR), datasets (e.g., USCDI), and clinical terminologies (e.g., LOINC, SNOMED CT, RxNorm). |
Examples of Telestroke Software Implementation
Massachusetts General Hospital offers comprehensive telestroke and teleneurology programs to community hospitals. Now, over 95% of consultation requests are answered within five minutes. Clinicians in remote hospitals report that MGH neurologists’ consultations improve decision-making confidence and allow treating 71%-88% of emergency telestroke patients locally.
SA Health, Australia, implemented a cloud-based telestroke platform to gather vital health information from stroke patients and provide virtual consultations. As a result, it reduced unnecessary hospital-to-hospital transfers by 72%.
Should You Opt for a Custom Telestroke Software?
Answer a few quick questions from our healthcare IT consultants to determine whether you need a custom telestroke solution.
Do you require high telestroke software convenience for stroke consultants and ER teams?
Do you have a complex IT environment or legacy apps that need to be seamlessly integrated with the telestroke software?
Do you want to automate operations for telestroke program administration, case reporting, reimbursement, etc.?
Do you need a specialized app for patient rehabilitation?
Do you plan on monitoring stroke patients’ vitals using connected medical devices or sensors?
Do you want to implement advanced telestroke software functionality? For example, medical image assessment using AI, VR-based surgery planning using MRI or CT-based 3D modeling, etc.
Tell us more about your needs
Please answer at least one question to help us better understand your business objectives.
A ready-made app may be the best fit for you
Based on your answers, an off-the-shelf telemedicine platform will suit the stroke care needs of your organization. ScienceSoft’s healthcare IT experts are ready to help you choose and implement the best-fitting software.
It’s best to opt for a custom telestroke solution
It seems that custom telestroke software is more suitable for your needs. ScienceSoft’s team is ready to help you define the necessary features, design a robust architecture, and develop a reliable telestroke solution.
Telehealth Software for Stroke Care by ScienceSoft
Holding ISO 13485 certification, ScienceSoft creates secure telestroke software in full compliance with the requirements of the FDA and the Council of the European Union.
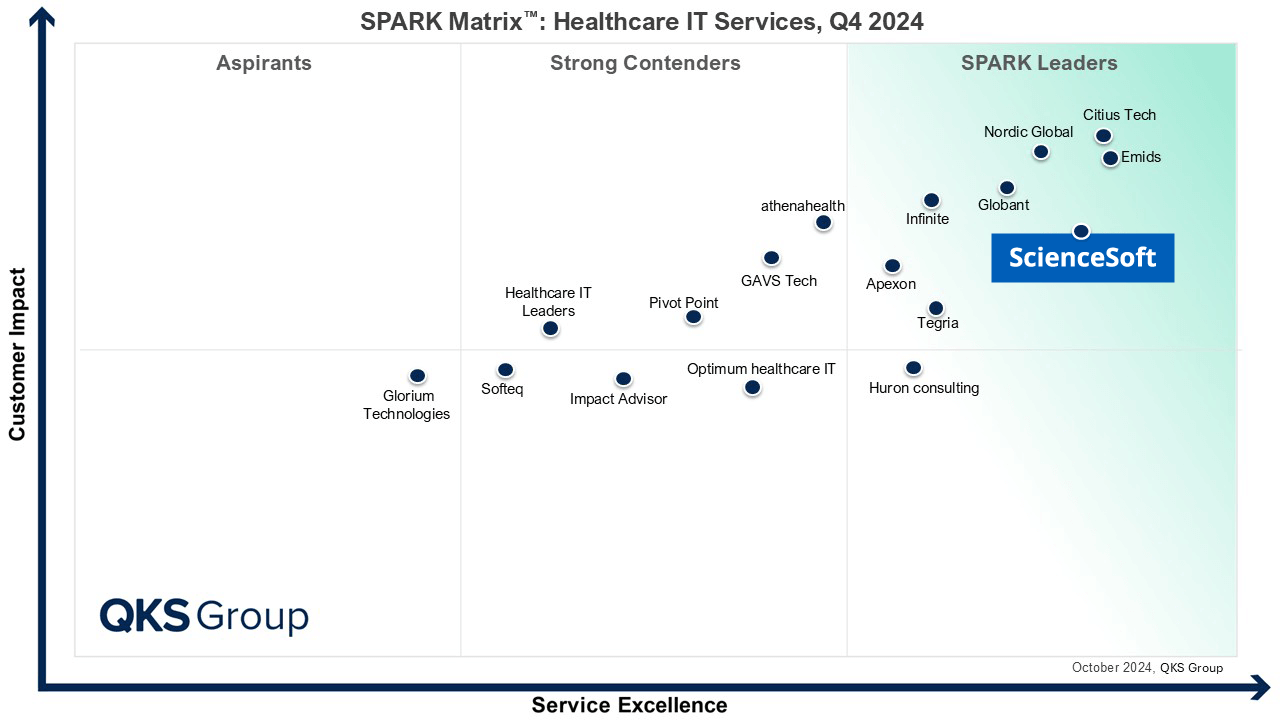
Featured among Healthcare IT Services Leaders in the 2022 and 2024 SPARK Matrix
Recognized for Healthcare Technology Leadership by Frost & Sullivan in 2023 and 2025
Named among America’s Fastest-Growing Companies by Financial Times, 5 years in a row

Top Healthcare IT Developer and Advisor by Black Book™ survey 2023
Four-time finalist across HTN Awards programs

Named to The Healthcare Technology Report’s Top 25 Healthcare Software Companies of 2025

HIMSS Gold member advancing digital healthcare
ISO 13485-certified quality management system
ISO 27001-certified security management system
About ScienceSoft
ScienceSoft is an international IT consulting and software development vendor since 2005 in healthcare IT. Being ISO 13485-certified to design and deliver medical software according to the requirements of the FDA and the Council of the European Union, ScienceSoft advises on the implementation of telehealth solutions for stroke care and develops software for rapid and accurate stroke diagnosis and treatment. Our mission is to drive your project success despite time and budget constraints, as well as changing requirements.