Artificial Intelligence for EHR
Use Cases, Costs, Challenges
Since 1989 in AI software development, ScienceSoft helps healthcare providers enhance EHR and EMR systems with AI to improve care quality and efficiency.


The Essence of AI Technology in EHR
When embedded in EHR, AI analyzes health records to improve diagnostic accuracy and predict complications. Quality-of-life AI features (NLP, image recognition, smart input suggestions) enhance operational efficiency and streamline patient records management for physicians and nurses.
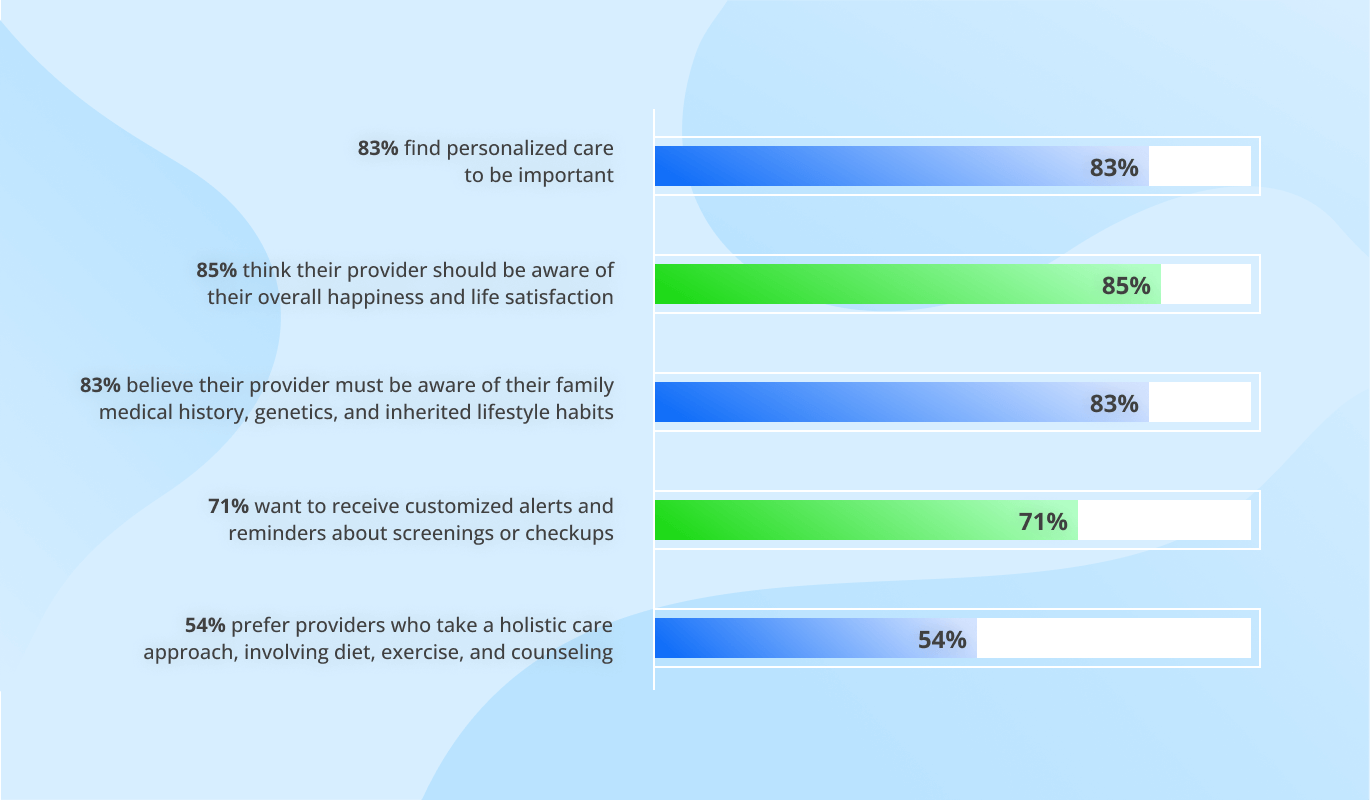
Market Overview and Benefits
The healthcare AI market was estimated at $26.57 billion in 2024 and is projected to reach $505.59 billion by 2033, growing at a CAGR of 38.81%. The need to improve complex and inefficient EHR workflows and get valuable insights from historical patient data drives the demand for AI-powered EHRs.
How does AI improve EHR?
|
Speeds up patient record management thanks to convenience features (e.g., speech recognition, AI suggestions for data entry). |
Lifts the load of administrative tasks off physicians and nurses by automating routine processes (e.g., appointment scheduling, clinical documentation), leaving more time for direct patient care. |
|
Improves patient care quality and consistency thanks to more cohesive records, AI-enhanced treatment planning, and more. |
Provides diagnostic assistance with an accuracy of up to 98.7%. |
AI-Powered Capabilities for the EHR
Generative AI can turn patient encounter conversations or post-visit narratives into draft documentation and structured EHR entries. Using speech recognition and clinical language models, AI scribes can identify symptoms, diagnoses, medications, allergies, procedures, and orders; place them in the appropriate note sections or data fields; and map them to standards such as ICD-10, CPT, SNOMED CT, and RxNorm. However, clinicians remain responsible for the review, correction, and sign-off before any content becomes part of the chart.
Chart intelligence
With generative AI, clinicians can navigate long, fragmented patient records using focused chart summaries tailored to the task at hand. AI copilots can gather recent events, active problems, medications, labs, imaging, referrals, and prior notes into concise pre-visit or in-visit views, generate timelines for specific conditions or episodes of care, and highlight conflicting or incomplete information that may require attention. This way, clinicians find relevant history faster and use it more consistently.
AI can support diagnostic work by turning patient history, symptoms, early clinical notes, images, and structured data into diagnostic hypotheses, clarifying questions, abnormality flags, and risk estimates. Because these capabilities influence clinical decision-making, they typically require a controlled implementation model: outputs should be transparent, grounded in source data, and reviewed by clinicians before use. More complex or less explainable use cases may need to be delivered as FDA- or CE-regulated products. As always, final interpretation and diagnosis remain the clinician’s responsibility.
During ongoing care, large language models (LLMs) can help summarize relevant patient context, surface applicable guidelines, explain why a recommendation may or may not fit the current case, and identify missing information that may need clarification before treatment proceeds. Predictive models can estimate the risk of complications, deterioration, non-adherence, or likely response to treatment based on clinical history, labs, medications, and other structured data. Rules-based and knowledge-based systems can check medication selections for interactions, contraindications, dosing issues, and guideline alignment using drug databases and clinical protocols.
Prior authorization support
LLMs can extract relevant diagnoses, prior treatments, test results, and clinical rationale from the record and turn them into draft authorization requests or medical necessity letters. Rules-based logic can then check those materials against payer-specific criteria, showing which requirements appear to be satisfied and which still need support. In higher-volume settings, predictive models may also help identify requests with a higher likelihood of delay, denial, or manual rework so teams can prioritize them earlier.
Billing and coding support
LLMs can review encounter documentation, suggest visit-level or procedure codes, and explain where the record may not fully support the billed service. Predictive models can help billing teams focus attention on claims that resemble past denials, undercoding patterns, or documentation-related exceptions. In parallel, rules-based validation can compare proposed coding against payer requirements, internal edit logic, and required documentation elements before submission.
Generative AI can support patient communication within EHR workflows by preparing and delivering structured messages tied to specific care events. This includes discharge instructions, follow-up reminders, test preparation guidance, and post-visit care instructions based on the documented plan. AI agents can also help collect structured patient inputs through pre-visit questionnaires, intake forms, or symptom check-ins, using conversational interfaces where appropriate, including voice-based interactions.
Operational optimization
Predictive models can be used to forecast no-shows, cancellations, workload spikes, or likely delays across scheduling, intake, referrals, inboxes, and follow-up queues. Process mining and anomaly detection can help identify where throughput breaks down, where handoffs are slow, or where work repeatedly stalls. Generative AI is more useful at the communication layer: turning these signals into readable summaries, exception views, or recommended follow-up actions for managers and frontline teams.

AI Medical Scribes in Daily Practice
In this interview, Hadeel Abu Baker explains how AI medical scribes support EHR workflows with faster note creation and less manual data entry. She also explains when human review is needed and how workflow design affects safe adoption.
How Much Does a Custom AI EHR Cost?
Key cost factors
- The intended scope and complexity of AI functionality.
- The required accuracy of ML algorithms.
- The data quality thresholds, number of data sources, and the volume of data to be stored and processed.
- The number and complexity of integrations with other solutions (e.g., patient portals).
- Security, UI, and UX requirements.
- Compliance-associated costs (e.g., alignment with the 21st Century Cures Act on standardized APIs and information sharing, FDA registration of SaMD functionality).
- Cloud services (e.g., ML tools), infrastructure, maintenance, and support costs.

On average, the costs of a full-fledged custom EHR system range from $120,000 to $800,000+. This includes AI features like virtual physician assistance and smart suggestions, as well as integrations with healthcare IT systems such as HIE and CRM.
Learn the cost of your AI EHR development project!
Get to Know the Cost of Your EHR Development Project
Please answer a few quick questions about your EHR requirements to help our healthcare IT consultants calculate your solution cost faster.
Thank you for your request!
We will analyze your case and get back to you within a business day to share a ballpark estimate.
In the meantime, would you like to learn more about ScienceSoft?
- Project success no matter what: learn how we make good on our mission.
- Since 2005 in healthcare IT services: check what we do.
- 4,200+ successful projects: explore our portfolio.
- 1,400+ incredible clients: read what they say.

Tech Stack to Employ AI for EHR
Since 2005 in medical software engineering, ScienceSoft recommends using the following technologies for AI-enabled EHR software development:
How to Tackle Challenges of AI Implementation for EHR
With AI-based EHRs, healthcare organizations can significantly improve the performance of the medical staff and reduce care costs while improving the value of care. Relying on 36 years of experience in AI software development, we know the benefits always come with technology challenges. Here, we list the most common of them and offer the solutions that proved to be efficient in practice.
Challenge #1: Ensuring AI outputs are accurate, complete, and grounded in patient data.
Even well-performing models may generate outputs that miss relevant details, overlook conflicting information, or rely on incomplete data.
Solution
In EHR workflows, accuracy issues are often caused by how the clinical context is retrieved and assembled before generation. Outputs may miss relevant details, overlook conflicting information, or rely on incomplete data if retrieval is not handled properly. Because of this, many solutions rely on retrieval-augmented generation (RAG), where the model generates responses based on patient-specific data retrieved at runtime.
The quality of outputs depends heavily on how the retrieval is organized. For example, if clinical notes are split into chunks that break logical context, the model may miss key relationships between findings. If retrieval relies on keyword matching, it may fail to surface clinically equivalent terms documented differently across providers. This is why semantic retrieval and careful context assembly often matter as much as the model itself.
In more complex scenarios (e.g., generating longitudinal summaries or combining multiple clinical signals), multi-step retrieval approaches can improve coverage, although they introduce additional latency and should be used selectively.
Challenge #2: Connecting AI to EHR systems without giving it excessive access or autonomy.
AI systems need to interact with clinical data and, in some cases, trigger downstream actions. Without clear boundaries, this can lead to broader data exposure than intended or to AI performing actions that were not explicitly designed or approved.
Solution
In simpler scenarios, where the AI needs access to a limited number of well-defined data sources or actions, explicit APIs are often the more predictable option. They allow providers to define exactly what data can be retrieved and which operations can be executed, which is especially important for write actions or workflows with compliance implications.
More flexible approaches, such as exposing tools through unified interfaces (including protocols like MCP), become useful when the AI needs to operate across multiple systems dynamically. However, this flexibility introduces additional complexity. The system must enforce stricter authorization, ensure that each tool is scoped appropriately, and prevent unintended combinations of actions.
It's better to start with tightly scoped integrations and expand only where there is a clear need for more dynamic behavior. This helps maintain control while still allowing the system to evolve toward more advanced workflows.
Challenge #3: Combining different AI approaches within a single workflow.
A common concern in EHR projects is whether LLM-based systems can be trusted to handle complex operations end to end. The hesitation usually stems from parts of the workflow that require precise calculations or validation based on strict rules, where LLMs are typically less effective.
Solution
ScienceSoft’s engineers recommend breaking every AI workflow down into smaller tasks and matching each task with the most suitable approach.
For example, a medication-related workflow may involve extracting relevant information from clinical notes, checking it against known contraindications, estimating patient-specific risks, and generating a human-readable explanation. These steps are better handled by different components: natural language processing for extraction, rule-based logic for deterministic safety checks, machine learning for risk estimation, and language models for text generation.
Treating a workflow as a composition of methods makes the system more predictable and easier to control. It also allows teams to optimize each step independently, balancing accuracy, latency, and cost.
Challenge #4: Keeping AI workflows secure and auditable without limiting their usefulness.
AI systems introduce new layers of data handling (prompts, retrieved context, and intermediate outputs) that are not always visible in traditional EHR architectures. This makes it harder to control data exposure and maintain traceability.
Solution
A common risk appears at the retrieval and orchestration stages, where the system may pass more data to the model than necessary or pull information across encounters, providers, or timeframes without clear scoping. It increases the risk of unnecessary PHI exposure and makes outputs harder to interpret and audit.
To address this, the system should limit what data can be retrieved and passed to the model based on the user role, task, and workflow stage, not only system-level permissions. This is especially important in RAG-based setups, where retrieval effectively defines what the model “knows” in a given interaction.
Another common gap is traceability. If only final outputs are logged, it becomes difficult to understand how a result was produced: what data was retrieved, what inputs were used, and what transformations happened along the way. Capturing inputs, retrieved context, and outputs as part of a single trace makes it possible to audit AI behavior and investigate issues when they occur.
It is also important to treat AI risks as an extension of existing security and compliance processes rather than a separate layer. This includes aligning with identity-based access controls (instead of shared API keys), applying existing monitoring and audit policies to AI interactions, and introducing additional safeguards for workflows that involve broader data access or higher-impact actions.
AI Readiness Check: Is your business ready for AI?
Answer 5 quick questions to assess your readiness and get tailored recommendations.
Do you have a specific task or process you want to improve with AI?
Do you have examples of how the process works today and what results you expect?
Do you already collect data that could be used for AI or automation?
Is your data easy to access and use (e.g., stored in systems rather than scattered across files)?
Do you have a way to measure success (e.g., time saved, cost reduction, accuracy)?
Tell us more about your AI situation
Please answer at least three questions to get results.
You’re at the early stage of AI readiness
Your current setup may not support effective AI implementation yet. The main gaps are likely related to data availability, structure, or process clarity, which are essential for building reliable AI solutions.
Before starting AI development, focus on:
-
organizing and centralizing your data
-
defining clear use cases
-
ensuring your systems can provide data automatically
You’re on the right track, with some gaps to address
You already have key components for AI adoption, but some limitations may affect the speed or quality of implementation.
To move forward efficiently, you may need to:
-
improve data quality or accessibility
-
refine your use cases and expected outcomes
-
ensure smooth integration with your systems
You’re ready to implement AI solutions
Your setup indicates strong readiness for AI development. You likely have the data, infrastructure, and clarity needed to move forward efficiently.
The next step is to validate your approach with a pilot or proof of concept and define the optimal architecture for your solution.
Robust Architecture for an AI-Enabled EHR System
Below is a sample architecture that illustrates how AI capabilities can be embedded into an EHR environment. It reflects a cloud-first setup designed to support end-to-end clinical and operational workflows, including documentation and chart navigation, clinical decision support and medication safety, as well as coding, revenue cycle, and quality or registry reporting. The example uses Microsoft services, but the same architectural pattern can be adapted to other cloud platforms and tools. It can also be adjusted to support a narrower or broader set of AI use cases.
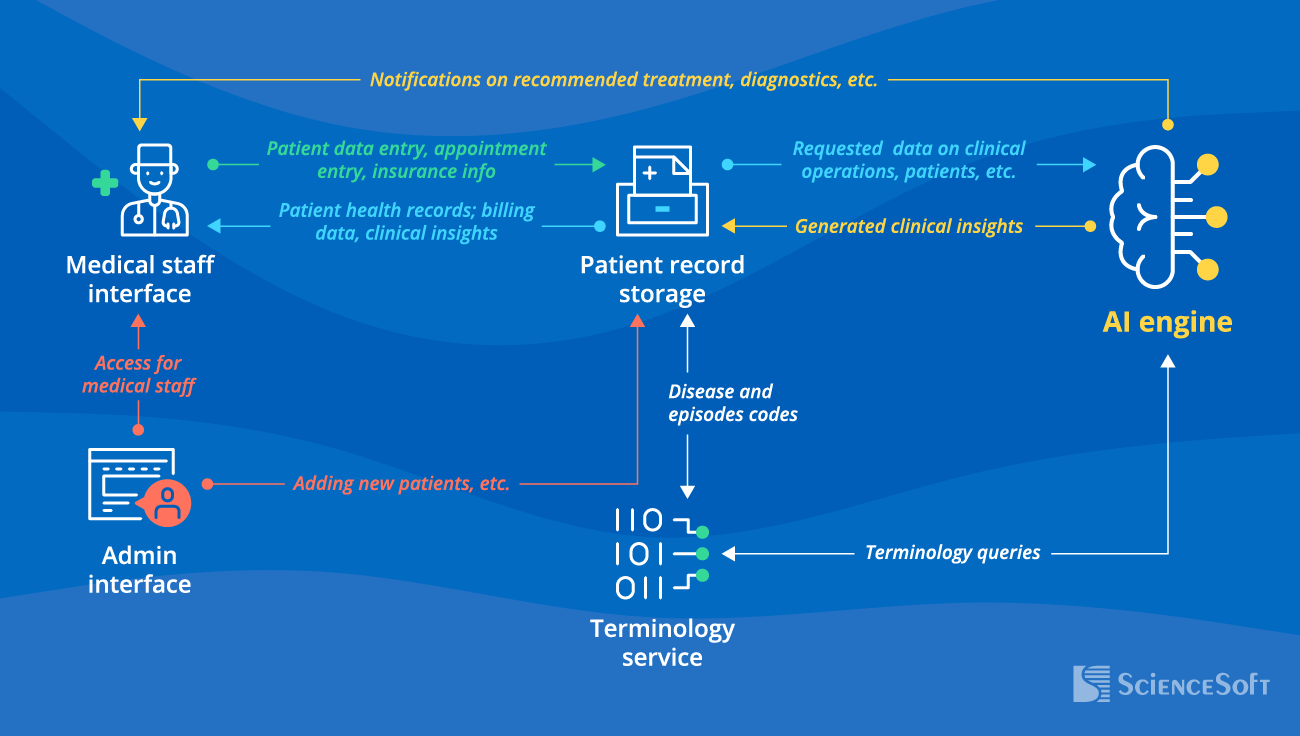
In the reference architecture, AI functionality is organized around separate workflow services rather than a single monolithic component. For example, documentation and summaries, clinical decision support, and billing workflows are handled independently. This separation makes it easier to control AI behavior, apply different validation rules, and introduce or remove capabilities without affecting the rest of the system.
To generate reliable outputs, the architecture combines large language models with retrieval and context management. The context and prompt engine keeps track of the active patient, encounter details, and task so that AI operates on the correct record and reflects the current workflow stage. At the same time, the retrieval-augmented generation (RAG) orchestrator pulls relevant clinical data from underlying sources such as EHR records, prior notes, lab results, imaging, and guideline repositories to provide the necessary context for each request. All AI responses are grounded in this data and linked back to source records, so clinicians can trace how a summary or suggestion was produced.
Different types of data are stored and processed separately depending on their role. Structured clinical data is managed through FHIR-based services, unstructured documents are stored in object storage, and operational or session data is handled in low-latency databases. This separation reduces contention between workflows, improves performance, and supports both real-time AI use and downstream analytics.
Human oversight is built into all high-impact steps. AI-generated outputs always appear as drafts or suggestions, with rule-based safety validation applied before they reach the user. Actions such as updating records or triggering downstream processes require clinician review and approval.
Security and compliance controls apply across all layers. Identity and access management restricts who can view or modify data, encryption protects information in transit and at rest, and monitoring services maintain a full audit trail of inputs, outputs, and user actions. This ensures that AI-supported workflows remain traceable and aligned with healthcare regulatory requirements such as HIPAA and HITRUST.
I always recommend integrating an EHR with your revenue cycle management system, practice management software, HIE software, a CRM, medical imaging software, a laboratory information system, a patient portal, or a telehealth app, using FHIR APIs aligned with USCDI.
It is especially important when you build an AI engine since it requires access to the most recent and relevant data from the connected systems to make correct decisions regarding patient care, diagnostics, follow-up examinations, and more.
ScienceSoft as a Trusted Partner for Healthcare AI Implementation
- Since 1989 in AI consulting and implementation services.
- Since 2005 in engineering custom solutions for the healthcare sector.
- Medical IT, compliance, and clinical leadership consultants with 5–20 years of experience.
- Principal architects with hands-on experience in designing complex clinical intelligence systems and driving secure implementation of AI technologies.
- Data scientists with a vast track record in designing custom AI/ML models for healthcare, including diagnostics and clinical decision support.
- 45+ certified project managers (PMP, PSM I, PSPO I, ICP-APM) with experience in large-scale projects for Fortune 500 companies.
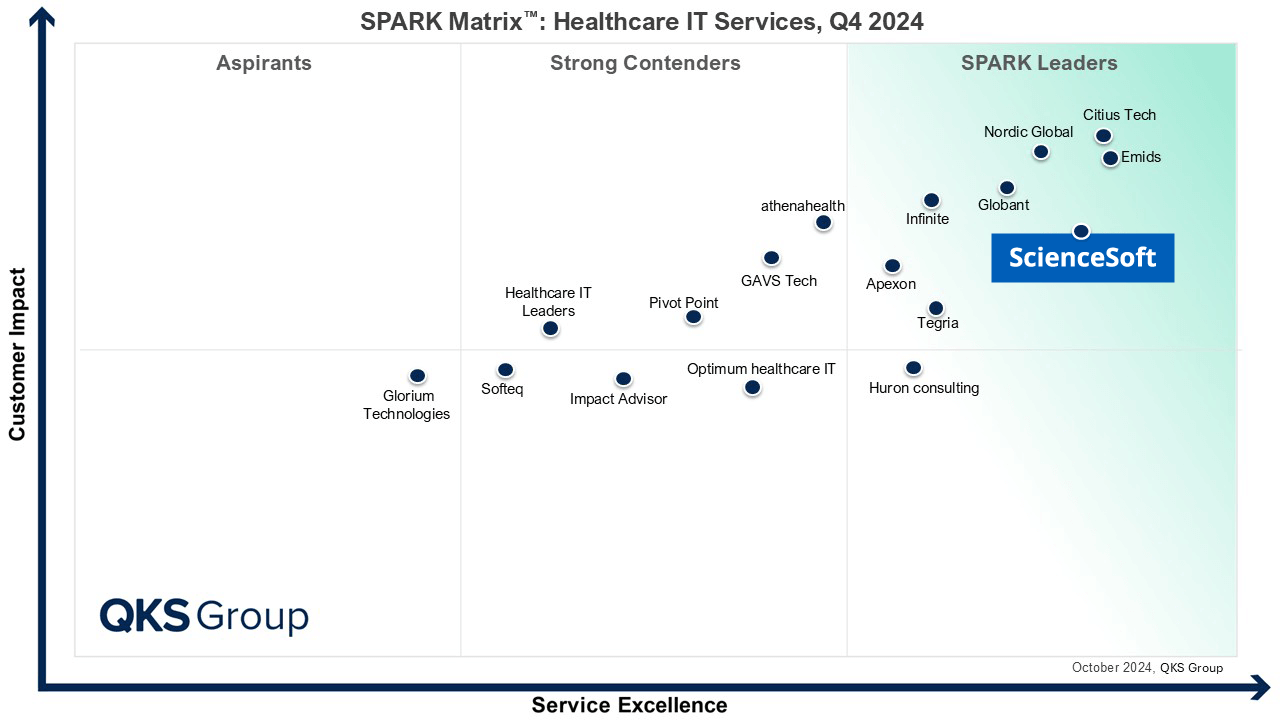
Featured among Healthcare IT Services Leaders in the 2022 and 2024 SPARK Matrix
Recognized for Healthcare Technology Leadership by Frost & Sullivan in 2023 and 2025
Named among America’s Fastest-Growing Companies by Financial Times, 5 years in a row

Top Healthcare IT Developer and Advisor by Black Book™ survey 2023
Four-time finalist across HTN Awards programs

Named to The Healthcare Technology Report’s Top 25 Healthcare Software Companies of 2025

HIMSS Gold member advancing digital healthcare
ISO 13485-certified quality management system
ISO 27001-certified security management system
Take a First Step Toward Your AI-Powered EHR with Experts
With over 150+ winning IT projects for the healthcare industry, ScienceSoft implements cutting-edge EHR software with AI capabilities for records management, diagnostics, and treatment.
Insights From ScienceSoft's Healthcare IT Experts
About ScienceSoft
A global IT consulting and software development company, ScienceSoft was founded in 1989 and worked with AI ever since. Now, with a team of seasoned healthcare IT consultants and developers, ScienceSoft designs and develops EHR solutions with best-in-class advanced features.