AI-Powered Medical Devices
Architecture, Functionality, Use Cases
ScienceSoft leverages 36 years of experience in AI software development and 20 years in healthcare IT to create AI-enabled medical software that our clients can rely on.


AI-Powered Medical Devices: The Fundamentals
AI-based medical devices comprise two main categories: medical devices connected to AI-enabled cloud software and AI-supported applications that function as medical devices. In both cases, artificial intelligence can significantly improve healthcare outcomes by assisting doctors with diagnostics, treatment planning and management, complications prediction, drug prescription, dosage calculation, and more.
Market Overview
By 2033, the AI/ML-powered medical devices market is expected to reach $255.76 billion.
The vast majority of devices authorized as of 2024 are in radiology, followed by cardiovascular, neurology, hematology, gastroenterology/urology, ophthalmology, and anesthesiology.
How AI-Powered Medical Devices Work
Architecture
This is a sample architecture of an AI-supported SaMD solution recommended by ScienceSoft’s consultants.
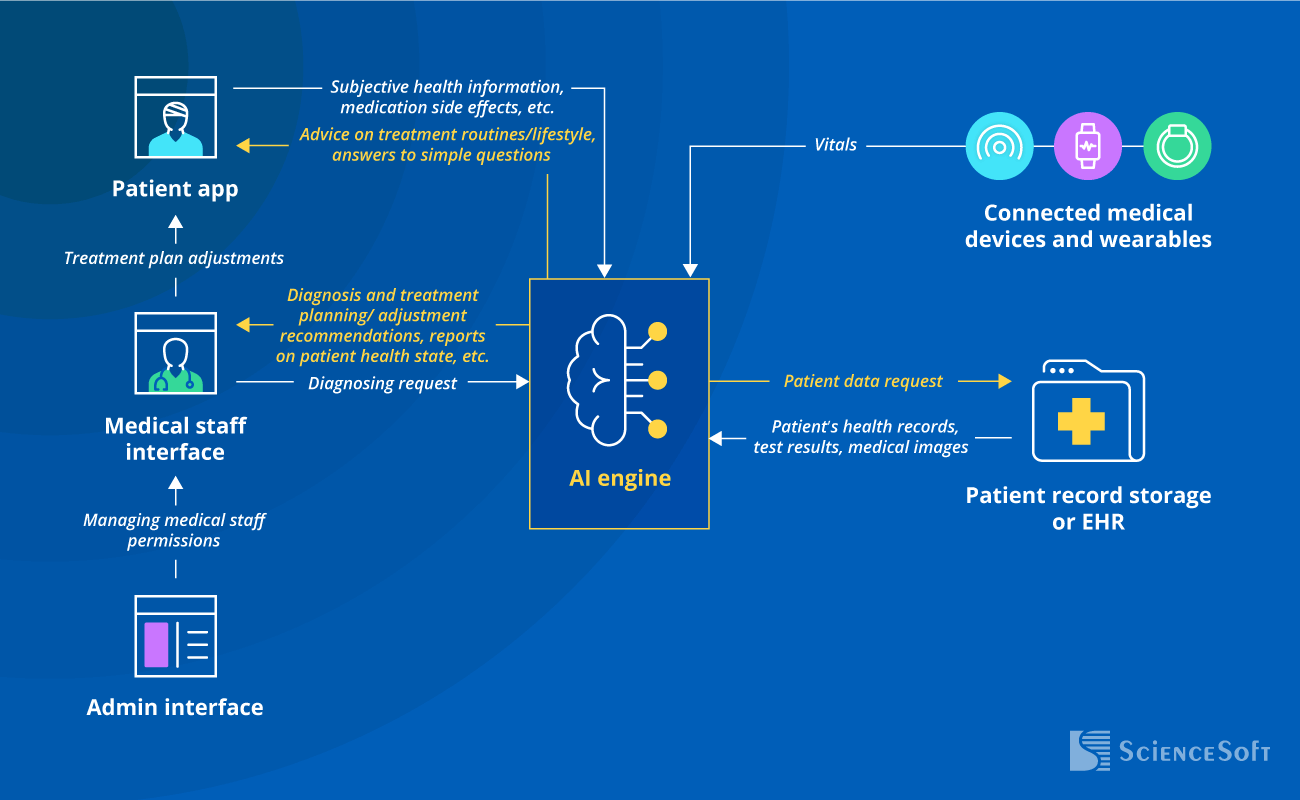
Use cases
AI analysis of clinical data (laboratory results, clinical notes, or medical images) helps identify conditions that may not be immediately obvious to the human eye. Machine learning and computer vision models can detect patterns or abnormalities in imaging and physiological data. Language models can then organize patient history and test findings into clear clinical interpretations with links to source data, reducing time spent reviewing complex cases.
AI-enabled CDS tools can help tailor treatment plans by combining patient-specific data with evidence-based medical knowledge. Predictive models estimate how a patient might respond to different therapies or identify potential risks, while large language models (LLMs) summarize relevant findings, highlight trade-offs, and present supporting evidence in a structured, easy-to-review format.
Remote care delivery
When integrated with connected devices and patient apps, AI-enabled SaMD can support semi-autonomous care delivery outside the clinic. Based on predefined logic and ML-predicted thresholds, the system can initiate direct actions, e.g., triggering an insulin dose if blood glucose spikes. In physical therapy, computer vision models can assess whether a patient is performing exercises correctly and provide real-time feedback. Meanwhile, LLMs can enable software accessories to “talk” to patients to check and record symptoms, offer clinician-approved explanations, and more.
Medication efficiency monitoring
AI-powered software can assess how well a treatment is working by analyzing data from smart medication devices (e.g., pill bottles, injection pens) alongside clinical outcomes, lab results, and patient-reported symptoms. Machine learning models can identify non-response patterns or adherence issues and suggest possible changes in dosage or formulation. GenAI can collect patient feedback to help determine whether issues are pharmacological or behavioral, summarize usage trends, and draft outreach messages with reminders or new instructions.
Monitoring and early warning
AI can continuously monitor patient data to detect early signs of deterioration or emerging complications. Predictive models can flag critical changes in trend data or detect anomalies that might signal decompensation, often before overt symptoms appear. LLMs then summarize what triggered the warning, why it matters, and what next steps might be appropriate. They can also reduce alarm fatigue by helping prioritize alerts and prepare context-aware escalation messages.
While not a replacement for professional therapy, properly designed and validated AI tools can act as therapeutic companions offering meaningful support, particularly in underserved settings. LLMs can suggest CBT-based exercises, guide journaling prompts, or help patients reflect on stressors in a non-clinical setting. AI may also assist with risk screening and escalation by recognizing key phrases or behavioral patterns that suggest distress.
While many healthcare providers remain cautious (and rightly so) about the use of generative AI in regulated medical software, large language models (LLMs) can play a meaningful and safe role when applied to the right layer of functionality. They are especially effective at handling unstructured inputs, reasoning across context, and turning complex clinical data into human-readable explanations. Core medical logic, including diagnosis estimation, treatment optimization, and early warning, should still rely on traditional machine learning (ML) and computer vision models that are specifically trained for narrowly defined clinical tasks. And in some cases, you don’t even need AI: deterministic rule-based algorithms work best for functions that require strict consistency, such as enforcing thresholds, triggering alerts, or validating actions against predefined constraints. So, when introducing AI, you should choose an appropriate model for each task type: traditional ML for risk estimation and forecasting, rule-based logic for controlled execution, and language models for summarization and dialogue.
Clinical AI capabilities
Descriptive analytics
Detection of anomalies, real-time changes, and long-term patterns across physiological signals.
Predictive modelling
ML-based risk estimation and outcome forecasting based on vitals, lab results, and other structured clinical data.
Prescriptive analytics
Data-driven recommendations on next steps based on predicted outcomes, predefined rules, and clinical thresholds.
Computer vision capabilities for processing medical images (CT, MRI, ultrasound, etc.) and identifying abnormal areas or changes that may not be immediately visible.
Motion analysis
Analysis of movement patterns using video or motion sensor data to assess posture, gait, and exercise correctness in rehabilitation scenarios.
Natural language processing
Extracting data from written and spoken text, including clinical notes, patient responses, and voice interactions.
Generating textual or spoken summaries, explanations, alerts, and patient instructions based on clinical data.
Agentic orchestration
Performing autonomous actions within predefined rules and approval constraints: triggering alerts when safety thresholds are exceeded or pausing device operation in the case of abnormal readings.

Chest X-Ray AI Feature for SaMD
This short demo shows a diagnostic AI feature inside a SaMD product for chest X-rays. A clinician pulls the study from PACS, reviews probability-backed findings with heat maps, and exports a report draft in one click. The solution is built for 90% or higher diagnostic accuracy and roughly 30% shorter reads.
Technologies ScienceSoft Uses to Develop AI-Powered Medical Software or SaMD
Challenges and Concerns
Does my app need FDA approval?
According to FDA, software that is “unrelated to the diagnosis, cure, mitigation, prevention, or treatment of a disease or condition” is not a medical device. If a product is only dedicated to maintaining or encouraging a healthy lifestyle, it’s considered a general wellness product and, therefore, does not require submission to FDA.
Ensuring the accuracy of ML models.
As a first step, data scientists should ensure that data sets intended for ML model training are of high quality. This can be achieved by examining and cleaning the data to avoid erroneous, missing, or inconsistent values. During the ML model training, continuous testing for the credibility of the results is essential. At ScienceSoft, data scientists use, for example, dropout techniques and optimization algorithms to minimize the model’s output error.
Building a custom model from scratch can be quite costly.
Custom AI/ML models might be feasible in case of, for example, medical diagnosing where precision and security are crucial. For more common tasks such as speech recognition, ScienceSoft’s data scientists suggest using pre-trained models. This will be a more cost-effective and faster to implement option than custom ML algorithms. Another solution would be tailoring and re-training an existing model.
How Much Does It Cost to Implement AI-Enabled SaMD or Software for Medical Devices?
When determining the cost of AI-supported medical software development, ScienceSoft considers the following factors:
- Functional scope and complexity defined by the software purpose (diagnostics, chronic disease management, etc.).
- Complexity of AI functionality (e.g., a chatbot that provides information upon request vs. image analysis system leveraging deep learning algorithms).
- Performance, scalability, security, and compliance requirements for the software.
- Number and complexity of integrations with other systems (EHR, doctor/patient apps, etc.).
- Deliverable type (PoC, MVP, a fully-featured solution).

From ScienceSoft’s experience, the cost of AI-powered cloud software for medical devices or AI-enabled SaMD may range from $200,000 to $650,000+. The former could be relevant for an individual AI-supported module (e.g., for drug dosage calculation), while the latter applies for end-to-end systems with several role-specific app integrations and complex algorithms dealing with diverse medical data.
Need a tailored cost estimation for your medical device software?













