Custom Rehabilitation Applications
Use Cases and Key Features
In medical software development since 2005, ScienceSoft advises on and helps create intuitive apps for patient rehabilitation.
Rehabilitation Apps In Brief
Rehabilitation apps employ telehealth, AI, remote patient monitoring, and other technologies to help patients restore cognitive and motor functions after traumas, surgeries, illnesses without visiting medical facilities. Rehabilitation apps enable remote therapy, monitor patient progress, and improve patient motivation, adherence, and health outcomes. Such apps are widely used for:
Healthcare providers value custom rehabilitation applications because they provide access to high-quality rehabilitation facilitated by connected medical devices, proprietary tech-enabled rehabilitation programs, AR, VR, and AI-based therapies.
Key Features of Rehabilitation Apps
How to Develop a Rehabilitation App
1
Analyzing the needs of a rehabilitation app's target audience.
2
Conceptualizing the app and designing a feature set for the target rehabilitation type (physical, cognitive, etc.).
3
Creating the regulatory compliance plan, considering HIPAA, GDPR, and MOHAP requirements (depending on the planned geography). If the app falls under the SaMD category (e.g., it provides tech-enabled rehabilitation interventions), it should be developed according to FDA or MDR requirements.
4
Designing the architecture, integrations, and software requirements.
5
Designing UX and UI of the app with a focus on accessibility for those with movement and visual impairments.
6
Iterative development and testing of the app.
7
Integrating the app with rehabilitation devices (e.g., smart gloves, biosensors).
8
Conducting pre-launch activities, e.g., preparing user training materials, HIPAA/GDPR audit, FDA 510(k) submission, and launching the app.
9
Supporting app users, maintaining, and improving the app.
Rehabilitation App in Real Life: Example by ScienceSoft
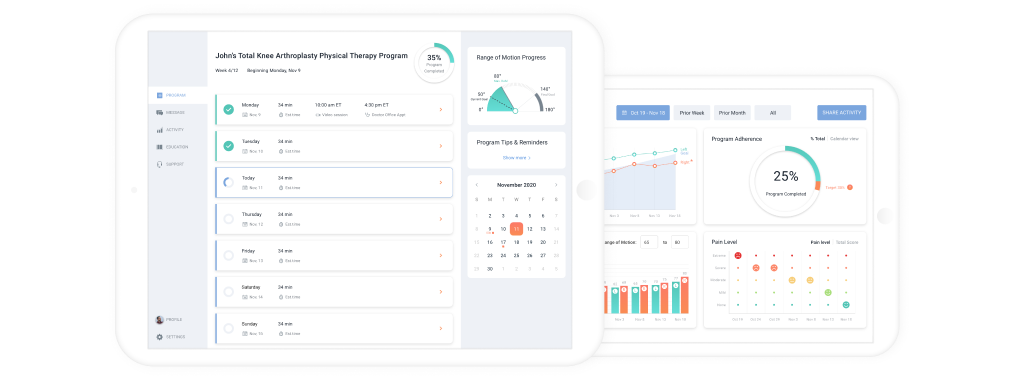
Client
Aklos Health, a US-based software product company.
Solution
A rehabilitation solution for home-based musculoskeletal physical therapy.
Project details
The solution consists of a web app for doctors, therapists and administrators and a cross-platform mobile application for patients.
Software features:
- Scheduling and conducting online video therapy sessions.
- Logging therapy progress.
- In-app messaging between doctors and patients, and more.
Project highlights
AI-driven assessment of therapy progress based on data from integrated range-of-motion sensors for knee joints monitoring.
