Software Modernization Services for Healthcare
With 21 years of experience in healthcare IT, ScienceSoft modernizes healthcare software without disrupting clinical workflows, interoperability, or regulatory compliance.
We don’t upgrade software in isolation. We redesign architectures, integrations, and data flows so modernized systems can support care delivery, remain stable in production, and be ready for continuous evolution.
Healthcare software modernization services help providers and life sciences companies evolve their legacy systems that have limited interoperability, scalability, and maintainability. The work typically involves re-architecting software, restructuring integrations, and improving data handling so systems can support new digital capabilities without introducing operational risk. Done well, modernization enables organizations to expand services, integrate new technologies, and adapt more quickly to regulatory and clinical changes. Our services support the modernization of healthcare systems while protecting care continuity and compliance.
Healthcare Software Modernization Pains We Handle
For healthcare providers
- Operational risk from aging systems. Legacy software fail more often and are harder to secure, increasing the risk of PHI exposure and care disruption.
- Limited interoperability. Older systems struggle with API-based integration and modern data standards such as FHIR.
- Clinical data growth exceeding system capacity. Expanding EHR, imaging, and operational data strains legacy storage and processing capabilities.
- Clinician workflow friction. Outdated UX and rigid workflows add clicks, rework, and delays to everyday care tasks.
- Systems are not ready for AI use. Many platforms lack the data pipelines, integration layers, and governance needed to deploy tools like clinical documentation assistants or call-center copilots.
For life sciences organizations
- Compliance and audit readiness exposure. Legacy systems often lack the traceability, controls, and reliable electronic records required for inspections.
- Validation is slowing system change. Rigid architectures and document-heavy validation processes make upgrades slow, costly, and high-risk.
- Quality and manufacturing bottlenecks. Legacy QMS and MES workflows slow down issue resolution, change control, and batch release.
- Disconnected business-critical systems. Limited integration across R&D, clinical, quality, manufacturing, and supply chain systems reduces visibility and coordination.
- Automation and AI initiatives blocked. Fragmented data and weak integration prevent reliable automation across safety, quality, and manufacturing workflows.
Our Healthcare System Modernization Services
Our healthcare software modernization services cover consulting, re-architecting, code and database updates, cloud migration, interoperability, security, and post-launch improvement.
Modernization consulting
We assess legacy healthcare software to reveal what stands in the way of modernization: brittle code and aging infrastructure, weak integrations, PHI handling risks, or workflow inefficiencies. From there, we can outline a phased, risk-aware modernization path that aligns upgrades with clinical realities and helps avoid unnecessary disruption.
Architecture modernization
We redesign system architectures during healthcare software reengineering to make them ready for growth while maintaining strong security and ease of maintenance. We can split monolithic architectures into microservices to ensure new components are easy to add without disrupting the functioning of the other components.
Software codebase and database modernization
We modernize legacy software and databases with no risk to critical workflows, data integrity, or compliance. We can convert outdated systems to modern technology stacks and update APIs through staged releases, so existing integrations keep working while new functionality is added. Together with our partner, Ispirer Systems, we can automate up to 95% of database migration.
We migrate healthcare software to cloud or hybrid environments with close attention to security and HIPAA compliance. Depending on your modernization goals, we can use rehosting, replatforming, or a cloud-native implementation. We plan the migration path and automate delivery to reduce manual errors, accelerate rollout, and support predictable releases.
Data and interoperability
We can prepare the data and storage infrastructure to integrate multiple healthcare systems, including legacy ones. This may include building a new data governance model, deduplicating data, mapping terminology (ICD, SNOMED, LOINC), and more. After that, we can build, test, and deploy a FHIR or HL7 data exchange solution.
UX and UI redesign
We can redesign software experiences around real clinical, administrative, and patient workflows. This can be aimed at making user journeys more intuitive, reducing human errors, or improving accessibility. Before rollout, we validate key workflows through prototypes and testing for target devices, including mobile.
Security and compliance alignment
We can help you check, validate, and improve PHI security in your connected systems. Our team can review your infrastructure and its controls, software architecture, and integrations. After that, we can address gaps in auditability, access control, and data protection to better protect PHI across systems.
Operations and continuous improvement
We help keep modernized software stable and prepare internal teams for post-go-live support. We monitor how the software performs in production, provide knowledge transfer and user training, and tune the solution where needed. We also watch key performance indicators to guide further improvement.
AI enablement for healthcare software
We can add AI capabilities to existing software without rebuilding them or making major architectural changes. Our team can integrate AI with internal systems by building RAG pipelines, custom MCP servers, and connectors, while putting guardrails in place for safe and compliant use. Where needed, we can also build and fine-tune custom SLMs.
I know “rehosting vs. refactoring” can sound like jargon, but the choice affects how safely you can modernize clinical and patient-facing systems.
Rehosting means moving the software to a new environment with minimal code changes. This is often the safest first step when you need to move many systems under strict downtime windows and keep integrations stable, because large migrations become much harder when you change code at the same time. Refactoring means changing parts of the code so the software is easier to update, runs faster, and fails less often. If an app already causes incidents or slows down staff workflows, rehosting usually moves the same problems to a new platform, so refactoring, or selective redesign, should be part of the modernization plan.
Re-architecting means changing how the software is built, for example, by splitting a large system into smaller parts so that a failure in one area does not take down everything. In healthcare, this step is usually needed when one busy area, like scheduling or portal login, forces you to scale the whole system, when releases are risky because everything is connected, or when outages in one module lead to disruptions in patient access or staff workflows.
Why Healthcare Organizations Choose ScienceSoft
- Since 2005 in healthcare IT, with over 150 successful projects for providers and life sciences organizations.
- Hands-on experience implementing HIPAA-compliant AI.
- 750+ IT professionals, including architects, business analysts, project managers, software and QA engineers, DevOps specialists, and data scientists. More than 50% of them are senior or lead specialists.
- Our Architecture Center of Excellence brings strong technical oversight and consistent architectural decisions to complex re-architecting, refactoring, and stabilization work.
- 45+ senior project managers in our Project Management Office help keep modernization programs on track, with tighter control over scope, timelines, risks, and cross-team dependencies.
- In-house compliance consultants, including Medical Doctors and HIMSS-certified specialists, are involved in discovery and solution planning.
- Proficiency in healthcare interoperability standards (HL7, FHIR, C-CDA, DICOM, and clinical coding and terminologies (SNOMED CT, LOINC, RxNorm, ICD-10, CPT, UCUM).
- Hands-on experience meeting HIPAA, HITECH, FDA, the 21st Century Cures Act, MDR, IVDR, GDPR, NCPDP, ONC, PDPL, and SAMHSA regulatory requirements.
- Partnerships with major platforms and migration tooling providers, including Microsoft, AWS, and Ispirer for accelerated database and software migration.
- Ready to sign a BAA (Business Associate Agreement) on demand.
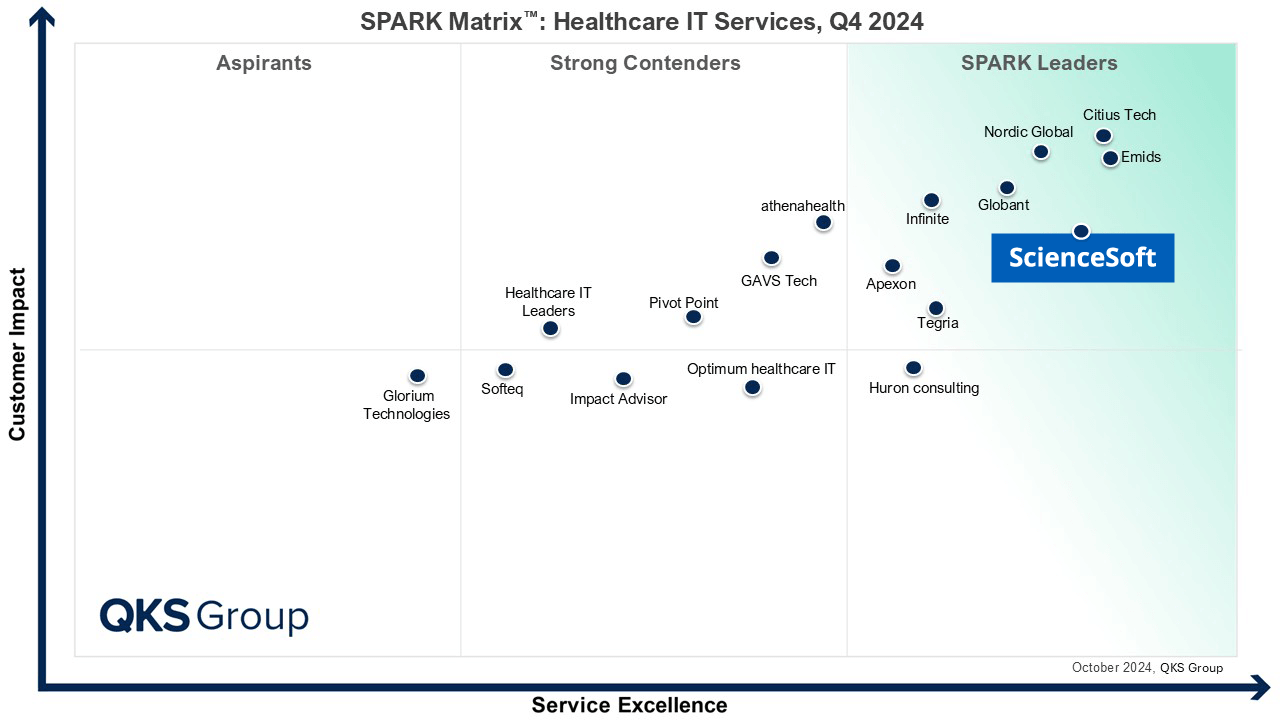
Featured among Healthcare IT Services Leaders in the 2022 and 2024 SPARK Matrix
Recognized for Healthcare Technology Leadership by Frost & Sullivan in 2023 and 2025
Named among America’s Fastest-Growing Companies by Financial Times, 5 years in a row

Top Healthcare IT Developer and Advisor by Black Book™ survey 2023
Four-time finalist across HTN Awards programs

Named to The Healthcare Technology Report’s Top 25 Healthcare Software Companies of 2025

HIMSS Gold member advancing digital healthcare
ISO 13485-certified quality management system
ISO 27001-certified security management system
Software We Modernize
Revenue cycle and operations
Technologies We Specialize In
Low-code development
Monitoring tools
Containerization
Infrastructure automation
CI/CD tools
Clouds
Generative AI
AI platforms and services

Agents and Orchestration
Traditional ML
Platforms and services




Frameworks and libraries
The Approach Behind Reliable Healthcare IT Modernization at ScienceSoft
Check how ScienceSoft keeps healthcare software compliant by aligning scope, testing, and change control with the required regulations and evidence expectations.
Discover how ScienceSoft approaches interoperability to ensure integrations remain predictable as systems evolve and interfaces are upgraded.
Learn how ScienceSoft manages security in healthcare projects, from architecture reviews and threat modeling to security testing and remediation planning.
Explore how ScienceSoft transfers knowledge and trains users in order to reduce dependency on individual experts and ensure high adoption.
Discover ScienceSoft’s approach to user convenience, including role-based flows, usability testing, and interface consistency that supports adoption across staff and patient users.
Understand ScienceSoft’s risk management workflow, from identification and scoring to mitigation planning with risk thresholds, ownership, escalation paths, and sample artifacts like risk matrices.
Learn how ScienceSoft plans collaboration models, aligns communication with stakeholder needs, and measures communication efficiency to avoid gaps that can derail delivery and change management.
See how ScienceSoft turns stakeholder input into an approved scope statement with traceability, explicit exclusions, and a structured process for handling scope changes.
Learn how ScienceSoft builds realistic estimates, anchored to validated scope, clear assumptions, and visible risks, with transparency on what the client is paying for.
What Drives Software Modernization in Healthcare

Sources: CHIME 2026, KLAS 2025









