Software Integration Services for Healthcare
In healthcare IT since 2005, ScienceSoft helps healthcare providers connect clinical, administrative, and partner-facing applications into stable, interoperable environments. Our architects build reliable, compliant, and scalable data exchange solutions with a focus on predictable delivery, minimal workflow disruption, and long-term IT stability.
Healthcare software integration services help providers establish reliable data exchange and coordinated workflows across EHRs, departmental software, patient apps, connected medical devices, and external partner systems. The result should be a secure, maintainable integration environment that supports FHIR and HL7. ScienceSoft supports the full integration lifecycle, from assessment and architecture design to implementation, testing, support, and evolution.
Healthcare Software Integration Scenarios We Handle
Adding new software
Connecting new software to the existing healthcare IT environment.
Connecting legacy software
Linking modern software with legacy clinical and administrative systems.
Supporting EHR replacement
Rebuilding interfaces and data flows when moving to a new EHR.
Cloud-to-on-prem integration
Connecting cloud software with on-premises healthcare systems.
Medical device integration
Bringing connected devices and diagnostic software into clinical and operational workflows.
Connecting with external partners
Enabling data exchange with labs, imaging partners, pharmacies, payers, HIEs, etc.
Modernizing the interoperability model
Redesigning interoperability architecture and governance, adopting new standards (e.g., FHIR).
Why Partner With ScienceSoft for Healthcare Software Integration
- 21 years in healthcare IT, delivering secure software, connected healthcare solutions, and long-term support for complex medical environments.
- 150+ healthcare clients worldwide and a portfolio that includes HIE platforms, EHR-first integrations, and software tested for compatibility with multiple EHRs.
- 750+ IT specialists on board, including architects, business analysts, engineers, QA specialists, MDs, and regulatory consultants; more than 50% are senior-level professionals.
- 20+ principal architects to design secure, HIPAA-compliant architectures and enable interoperability across in-house, partner, and legacy systems.
- In-house project management office support predictable delivery and controlled change management.
- Practical experience with healthcare data exchange standards, including HL7 v2/v3, FHIR, USCDI, CCDA, XDS/XDS-I, and NCPDP SCRIPT.
- Working knowledge of clinical terminologies and coding systems, including SNOMED CT, LOINC, RxNorm, ICD-10, and CPT.
- Hands-on experience with HIPAA, HITECH, the 21st Century Cures Act, and FDA considerations for connected medical devices.
- Ready to sign a BAA and support audit-ready delivery for regulated healthcare environments.
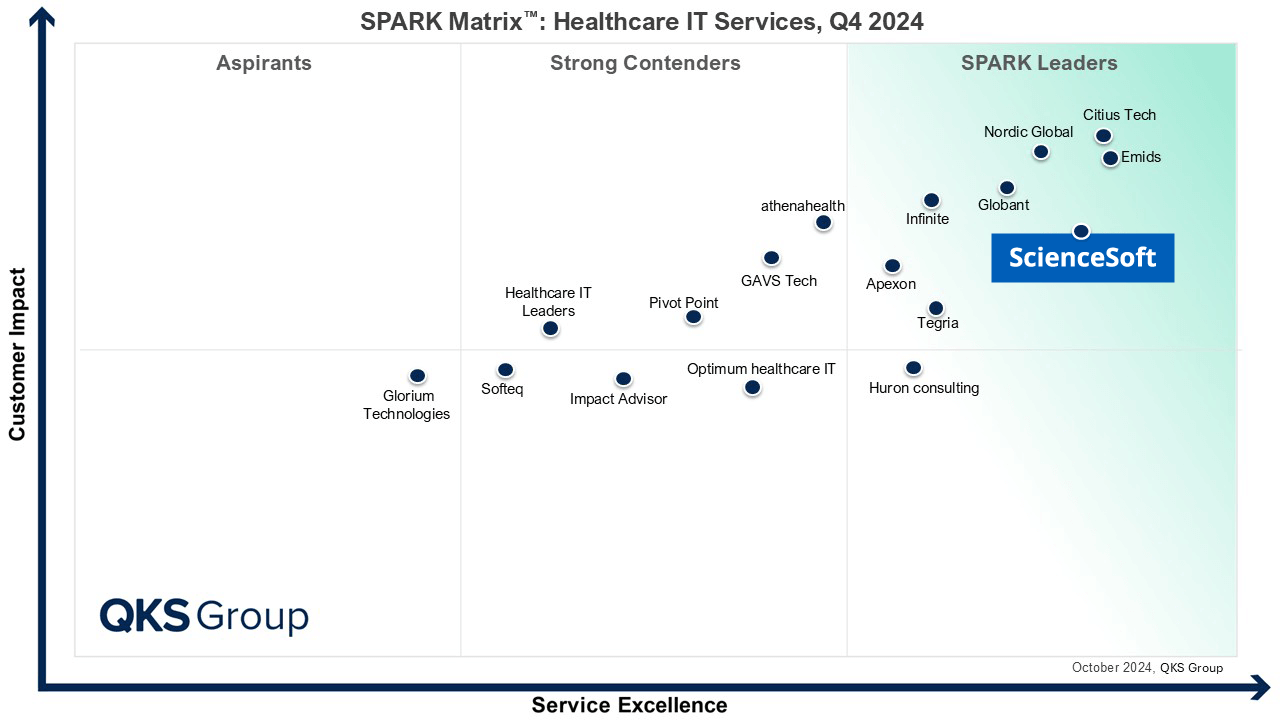
Featured among Healthcare IT Services Leaders in the 2022 and 2024 SPARK Matrix
Recognized for Healthcare Technology Leadership by Frost & Sullivan in 2023 and 2025
Named among America’s Fastest-Growing Companies by Financial Times, 5 years in a row

Top Healthcare IT Developer and Advisor by Black Book™ survey 2023
Four-time finalist across HTN Awards programs

Named to The Healthcare Technology Report’s Top 25 Healthcare Software Companies of 2025

HIMSS Gold member advancing digital healthcare
ISO 13485-certified quality management system
ISO 27001-certified security management system
Healthcare Integration Services by ScienceSoft
Integration strategy and scope consulting
We assess your software landscape, existing interfaces, workflow dependencies, and data exchange needs across clinical, operational, patient-facing, and device-connected systems. Based on this, we help define integration targets, priorities, risks, and a realistic roadmap, with recommendations suited to your care delivery model and operational context.
Interoperability architecture and interface design
We design integration architectures that fit your environment, growth plans, and governance needs. Depending on the case, we can use APIs, message-based exchange, event-driven patterns, middleware, or a hybrid approach. Our architects define consistent data flows, mapping logic, synchronization rules, security controls, and other interoperability design components needed for stable exchange at scale.
Integration implementation
We implement integrations across EHRs, departmental and patient applications, cloud and on-premises infrastructure, third-party systems, and connected medical devices. This may involve developing new interfaces, configuring middleware, changing data transformation logic, and modernizing legacy software. We can cover the entire interoperability ecosystem or only connect selected interfaces.
Integration validation
We validate integrated environments through interface testing, end-to-end workflow checks, data quality reviews, performance testing, and failure scenario testing. Our engineers can also verify that compliance-related controls and interfaces meet required healthcare interoperability standards and data specifications, then implement any necessary fixes and compose integration documentation.
Integration maintenance and optimization
We can help monitor integration health, resolve failures, improve performance, and support controlled changes in both new and existing integration environments. Our engineers can also coordinate updates across vendors and internal teams, helping keep the integrated environment stable in production and easier to support over time.
Need an estimate for your integration initiative?
We can examine your integration scenario, architecture needs, and delivery constraints and share an estimate with the main assumptions and cost drivers behind it. This is free and non-binding.
Healthcare Systems We Integrate
Integration Approaches We Apply
No single integration pattern fits every healthcare environment. ScienceSoft selects an approach based on the systems being connected, the standards and interfaces they support, the volume and direction of data exchange, and the amount of custom logic needed to ensure workflows run reliably.
|
|
Enterprise service bus (ESB) and interface engine This approach fits complex environments with many on-premises and legacy systems, such as multiple HL7 feeds, departmental applications, imaging, and billing platforms. It offers strong centralized control over routing, transformation, auditability, and protected health information flows, though it can become less agile as the number of changes and new consumers grows. Best for: Providers tying together many existing systems that were not built to work together. |
|
|
API-first integration This model works well when the environment needs modular, well-defined integrations across internal systems, partner applications, and patient-facing software. It supports stronger reuse, easier expansion, and granular control over authentication, authorization, rate limiting, and logging, which makes it a good fit for modern digital services and growing software ecosystems. Best for: Providers rolling out portals, apps, and partner-connected digital services. |
|
|
Integration platform as a service (IPaaS) This approach is suitable for cloud-heavy environments with many software-as-a-service (SaaS) platforms and frequent onboarding of new partners or services. It can speed up delivery through reusable connectors and standardized patterns, but the level of control depends partly on the platform vendor, especially in areas such as certifications, data location, and operating flexibility. Best for: Providers that need to link multiple vendor solutions (e.g., CRM, HR, billing, scheduling, telehealth) with less custom integration effort. |
|
|
Event-driven architecture This model is a strong fit for dynamic environments where many systems must react to changes in near real time without creating a large web of tightly coupled interfaces. It supports high throughput and resilience, but it also requires stronger engineering around event governance, observability, replay handling, and secure processing of sensitive healthcare data. Best for: Providers that need immediate reactions to data changes (e.g., in alert-driven care, remote monitoring). |
Do not redesign every legacy connection at once for the sake of integration. In many healthcare environments, existing integrations still support core workflows well enough and are better preserved until there is a clear operational or business reason to change them. The smarter approach is to assess dependencies, data flows, and affected workflows first, then redesign only the integration points that improve reliability, maintainability, scalability, or control. This usually helps reduce disruption, contain rollout risk, and focus investment where it brings real value.
Want to go deeper?
Explore ScienceSoft’s in-depth guide to legacy software integration to see how phased rollout, abstraction layers, fallback mechanisms, and incremental modernization help keep integrated environments stable over time.
Technologies We Specialize In
Low-code development
Monitoring tools
Containerization
Infrastructure automation
CI/CD tools
Clouds
Integration and data exchange technologies
Cloud integration services
Integration platforms and middleware
ScienceSoft’s Approach to Reliable Healthcare Software Integration
Review how ScienceSoft defines integration scope, covering approved requirements, interface boundaries, exclusions, constraints, and dependencies between connected systems.
Discover how ScienceSoft designs interoperability into healthcare software through standards-based interfaces, terminology alignment, data flow control, and early detection of transformation issues.
See how ScienceSoft treats legacy integration: dependency assessment, phased updates, abstraction layers, and resilient integration patterns that reduce disruption and support long-term maintainability.
Find out how ScienceSoft aligns integration delivery with healthcare regulations through validation planning, traceable decisions, controlled releases, and audit-ready project artifacts.
Review how ScienceSoft keeps integration documentation current, structured, and useful for delivery control, support handover, and further system evolution.
Understand how ScienceSoft reviews change requests, assesses their effect on interfaces and dependent workflows, and introduces updates in a controlled way.
Learn how ScienceSoft protects sensitive healthcare data through secure interface design, access controls, encryption, auditability, and project-specific safeguards.
Look into ScienceSoft’s risk management process, from identifying hidden dependencies and unstable interfaces to assigning owners and planning mitigation actions.
Explore the quality practices ScienceSoft applies to integration work, from interface validation and defect control to measurable quality indicators across delivery.
FAQ
Our EHR vendor and current systems limit what we can integrate. Can you work around that?
Healthcare environments nearly always come with system and vendor constraints, so we treat them as a design input. We check what your systems can already support, where standard interfaces are enough, and where additional engineering is justified. Based on that, we design an integration setup that works within vendor boundaries without letting those boundaries dictate the whole solution. This often means reusing stable existing interfaces where they already do the job, introducing standards-based APIs where they add flexibility, and adding an integration layer where it improves control and simplifies future changes.
What is the best way to support both legacy interfaces and newer API-based integrations in one environment?
We often design a mixed integration model: stable legacy interfaces continue to support mature workflows, while newer API-based connections are introduced where reuse, partner onboarding, or patient-facing functionality requires more flexibility. We define how those two layers will coexist, where transformations and routing should happen, and how monitoring will work across both. That way, clients can modernize their integration landscape without forcing a risky full reset.
When are direct interfaces enough, and when do we need a centralized integration layer?
Direct interfaces work well when only a few healthcare applications need to exchange a limited set of stable data. Typical examples are connecting a telemedicine app to an EHR, linking a practice management system with one imaging solution, or syncing appointment data between a patient portal and a scheduling system. A centralized integration layer is usually the better choice when a hospital or multi-site provider needs to connect many internal and external systems at once, for example an EHR, RCM software, care coordination tools, patient-facing apps, and partner organizations. In those environments, a shared integration layer reduces duplicated logic, improves monitoring, and makes new interfaces easier to add without destabilizing existing ones.
How do we handle identity matching and avoid duplicate or mislinked patient records?
ScienceSoft treats patient matching as part of the integration design. Our architects define which patient attributes will be used for matching, where identity checks should happen, how potential duplicates will be flagged, and when manual review is needed before records are linked or updated. Designing the matching rules, exception handling, and reconciliation logic from the start is how we keep that risk under control.
How much internal IT effort will be needed from our side during implementation and after go-live?
ScienceSoft’s team can take over most of the integration work, including architecture design, interface implementation, validation, and rollout planning. From your side, the most valuable input typically comes from system owners, workflow stakeholders, and decision-makers who can confirm priorities, review assumptions, and help resolve cross-team questions quickly. At the same time, we keep the process transparent for your IT team: provide structured hand-off, documentation, and knowledge transfer, and can train your specialists to support the integrations after go-live. ScienceSoft can also stay involved and continue with monitoring, support, and controlled changes.










