Long-Term Care (LTC) Software Development Services
ScienceSoft helps LTC operators modernize around their current core platforms by adding integrations, focused workflow modules, automated reporting, and stabilization for legacy components. Our principal architects design secure, interoperable infrastructures so that LTC teams can reduce rework, speed admissions and billing, and gain reliable operational insight.
Long-term care software development services deliver secure, workflow-fit applications and integrations that help LTC providers streamline care delivery, compliance reporting, and revenue workflows.
When ready-made software platforms can’t match real operations, reporting obligations, or multi-system environments, LTC organizations typically choose one or several custom implementation paths:
- Build a focused add-on module (e.g., eMAR, incident management, or family portal) to remove the biggest bottleneck without replacing core systems.
- Add an integration hub that normalizes identities and data, connecting hospitals, pharmacies, labs, and payers with monitored write-back flows and retries.
- Automate CMS reporting for nursing homes, SNFs, home health agencies, and hospices, with versioned templates, validations, and audit trails to avoid rejected submissions and rework.
- Create a shared data model and dashboards to track quality, staffing, and margin drivers across facilities, branches, or programs daily.
Why Choose ScienceSoft for Your LTC Software Initiative
- 20+ years in healthcare software engineering, with 150+ projects delivered, including complex care operations and supporting ecosystems.
- Architecture & Solutions CoE with 20+ senior architects to de-risk architecture choices and integration designs in multi-site LTC ecosystems.
- In-house PMO uniting 45+ senior project managers to keep multi-site programs predictable through scope changes and phased rollouts.
- Healthcare interoperability expertise (HL7, FHIR/USCDI, X12) and an integration-by-design approach to keep data flows auditable and stable.
- Experience applying medical terminologies and code sets, including ICD-10, CPT/HCPCS, SNOMED CT, LOINC, RxNorm, NDC, UCUM, and NCPDP SCRIPT.
- Hands-on experience engineering HIPAA-ready software aligned to setting-specific regulatory obligations for SNFs (MDS, PBJ, SNF QRP), home health (OASIS-E2, HHVBP), hospice (HOPE, HQRP), and assisted living (state licensing requirements).
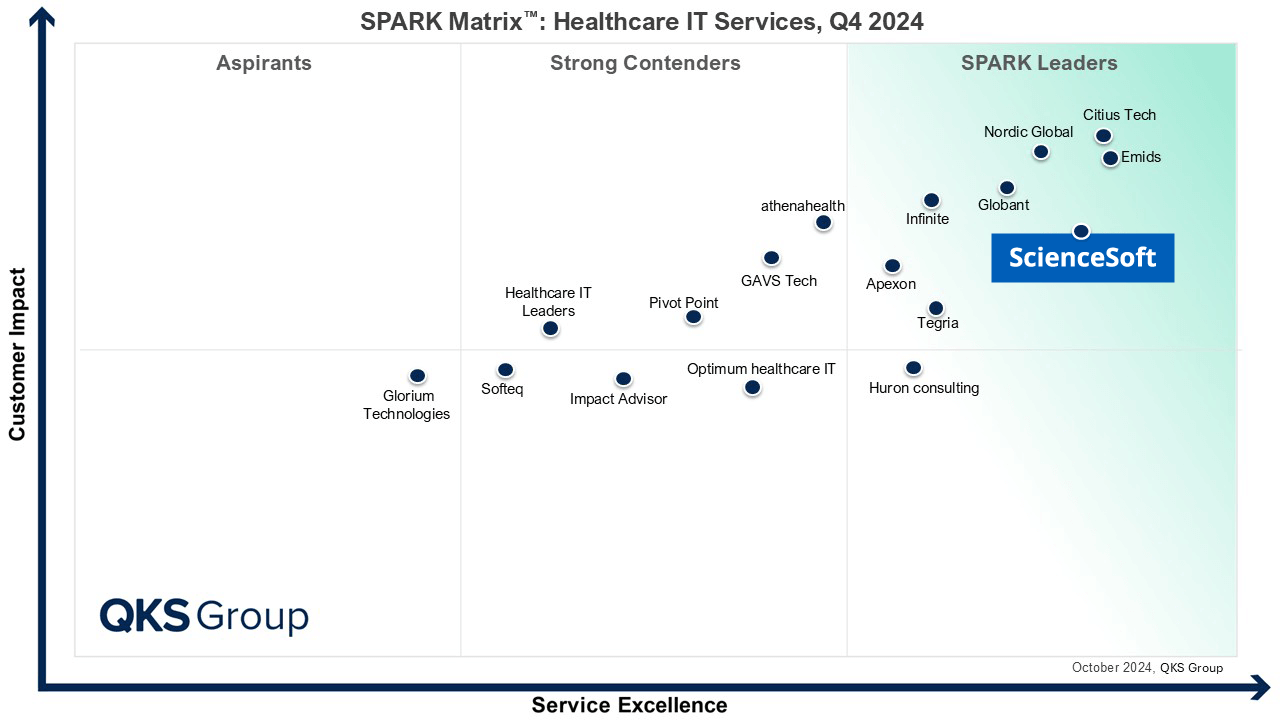
Featured among Healthcare IT Services Leaders in the 2022 and 2024 SPARK Matrix
Recognized for Healthcare Technology Leadership by Frost & Sullivan in 2023 and 2025
Named among America’s Fastest-Growing Companies by Financial Times, 5 years in a row

Top Healthcare IT Developer and Advisor by Black Book™ survey 2023
Four-time finalist across HTN Awards programs

Named to The Healthcare Technology Report’s Top 25 Healthcare Software Companies of 2025

HIMSS Gold member advancing digital healthcare
ISO 13485-certified quality management system
ISO 27001-certified security management system
LTC Solutions We Build, Maintain, and Evolve
ScienceSoft provides long-term and post-acute care (LTPAC) software development services for operators that need full-scale solutions or workflow-fit extensions around core platforms.
LTC care delivery and safety management
Electronic visit verification systems
Nurse call systems
Incident reporting and risk management systems
Infection surveillance systems
LTC operations and financial workflows
Engagement and remote care
Interoperability, data management, and analytics
Healthcare integration engines (HL7/FHIR interfaces)
Services ScienceSoft Offers for Long-Term Care Operators
Technology and IT architecture consulting
ScienceSoft helps LTC providers plan and de-risk software modernization, extension, replacement, and new implementation initiatives. Our team can map operational workflows against payment, reporting, and quality requirements (e.g., MDS and PDPM for SNF software), assess the current IT landscape, and recommend pragmatic architecture options with clear cost, timeline, compliance, and rollout tradeoffs.
Custom development and evolution of LTC software
We design, build, and evolve LTC software, from full-scale solutions to targeted extensions for existing long-term care EMR/EHR and billing systems. To reduce risk, we usually begin with a thin-slice pilot that tests essential workflows with real users. From there, we support stable releases and phased rollouts across sites, helping clients avoid disruption to daily operations.
LTC integration and data governance
We help LTC providers connect their core platforms to EHR and RCM systems, pharmacies, EVV vendors, and payers through controlled bidirectional interfaces. Our team delivers HL7, FHIR, and X12 integrations with identity matching, deduplication, and a unified data model so data can move cleanly between systems and support reporting, analytics, and dependable write-back.
Legacy LTC software modernization and stabilization
ScienceSoft modernizes legacy LTC software to keep resident management, care delivery, reporting, and billing workflows stable and available at scale. We help reduce technical debt and improve performance and usability without disrupting the live platform. Our engineers control release risk through dependency mapping, phased delivery, and fallback paths, and can re-platform to the cloud when it makes business sense.
Security and compliance engineering for LTC software
ScienceSoft’s engineers can implement ePHI protection across the core EHR, connected modules, and integrations, set up security monitoring and alerts, and close gaps in access control, audit logging, and encryption. As a result, our clients receive the documentation and test evidence needed to support HIPAA risk analysis, remediation planning, go-live approvals, security audits, and technical due diligence during acquisitions.
ScienceSoft can set up DevOps (SecOps) for LTC software to help providers keep systems stable, secure, and resilient after go-live. We implement monitoring, alerting, and performance tuning, and establish incident-response runbooks, backup procedures, and recovery drills. For long-term partnerships, we can provide SLA-based maintenance, security updates, safe releases, and multi-facility support.
Low-code engineering for cost-efficient LTC apps
ScienceSoft can use low-code platforms such as Power Apps to deliver LTC modules faster and at a lower cost than full custom development. Low-code is especially effective for back-office workflows, including intake, incident capture, and policy attestations across sites, and it gives teams greater flexibility to update forms, templates, and business rules without heavy IT support. Where workflows are high-load, public-facing, or integration-heavy, we complement low code with custom development.
Need to build, modernize, integrate, or extend your LTC software?
ScienceSoft’s healthcare IT consultants and architects are ready to scope the project and share an estimate.
Sample Architecture for an LTC Software Ecosystem
The diagrams below reflect the two operating models I see most often in LTC software initiatives: multi-facility care delivery for nursing home software and assisted living software, and mobile-first home-based care for home health and hospice settings. In both cases, the most realistic path is usually to keep the core systems that already run clinical and financial workflows and extend them with new modules and integrations.
These architectures can also support core-system replacement later on, because data continues to flow through one controlled integration layer even after you shift connections from the old core to the new one. That continuity helps reduce rework and lowers migration risk.
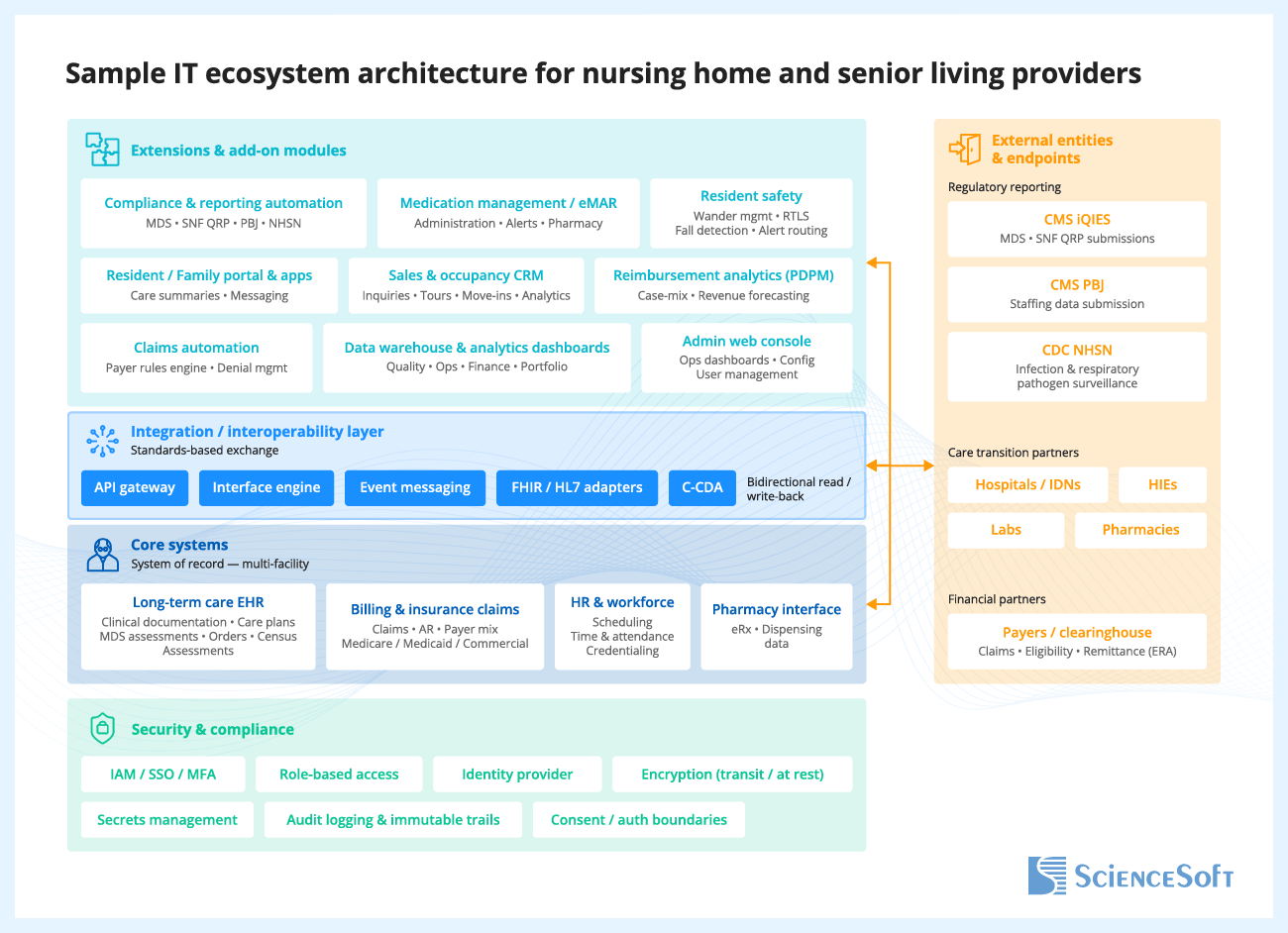
At the center of this architecture is a single interoperability layer that receives data from hospitals, health data networks, pharmacies, and payers, then validates, routes, and writes approved information into the care record, pharmacy interface, workforce tools, and revenue system. By using a single controlled exchange layer, providers can reduce re-entry in transitions, medication workflows, and claims processing. The same structured clinical and staffing data can also support MDS/RAI workflows and reporting, payroll-based staffing submissions, infection surveillance, and dashboards for reimbursement, quality, occupancy, and portfolio performance.
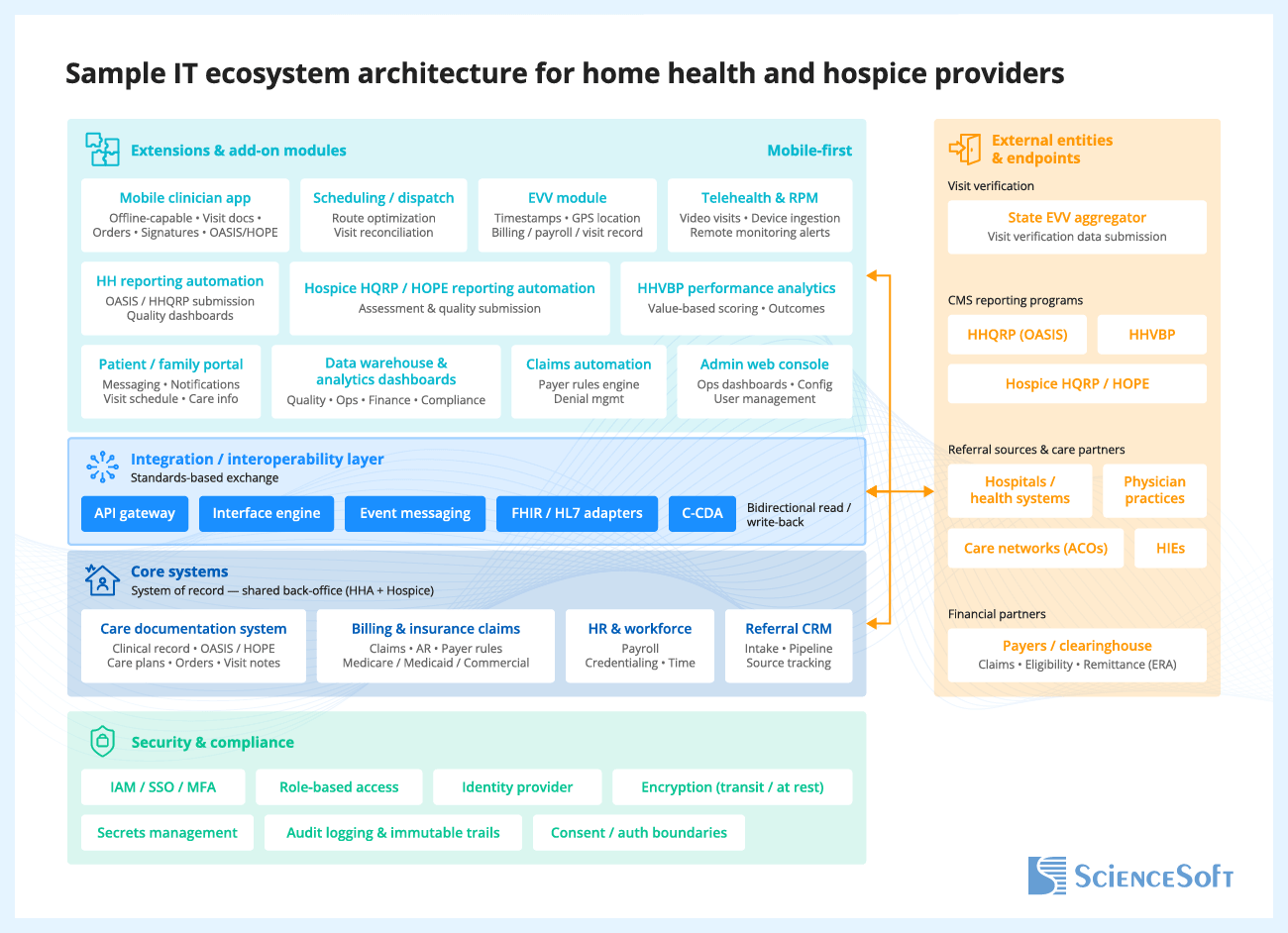
One controlled data flow connects mobile documentation, scheduling, visit verification, and telehealth services with the care record and billing systems. By writing visit notes, orders, timestamps, and location data back to source systems, this process helps reduce reconciliation work, billing delays, and payroll disputes. Routine workflow data is then reused to compile OASIS and HOPE datasets and support quality reporting, while referral and partner integrations help speed up intake. The same shared data layer gives managers a clear view of operations, finance, quality, and compliance.
How We Handle the Common Challenges in LTC Software Projects
As a software development company that works with long-term care providers, ScienceSoft shares proven approaches to resolving the recurring challenges we see in LTC systems.
Challenge 1. Fragmented care transitions due to weak system interoperability
Long-term care providers rarely run one unified system across clinical, operational, and financial work. Data arrives from hospitals, HIEs, pharmacies, and labs in mismatched formats and inconsistent identifiers. Staff re-enter data into the LTC EHR or RCM system and later fix conflicts. Transitions of care, referral intake, medication reconciliation, and billing evidence are the first to suffer. The result is slower admissions, higher documentation overhead, and avoidable quality and reimbursement risk.
Solution
Challenge 2. Documentation and regulatory reporting overload as CMS requirements evolve
Medicare-certified nursing homes and SNFs, home health agencies, and hospice providers must document care to satisfy clinical, billing, and quality programs, but CMS rules and forms change over time. If MDS, PBJ, OASIS, or HOPE datasets fail required-field validation, files are rejected, and staff must correct source records under time pressure. Rework drives overtime, disrupts claims, case-mix, and dashboard refresh cycles, and can trigger payment update reductions or compliance actions. In multi-site organizations, inconsistent templates and coding rules amplify variance, so corporate teams spend cycles normalizing data instead of improving care operations.
Solution
Challenge 3. Workforce workflows break across systems
Staffing, scheduling, documentation, and payroll often run in separate tools, so the same shift produces conflicting records. In home care, EVV mismatches can create exceptions that delay billing and force manual corrections. In nursing homes, auditable staffing submissions amplify the impact of data gaps. The result is wasted supervisor time, payroll disputes, slower cash flow, and weaker confidence in operational reports.






