Secure Messaging in Healthcare
Features, Integrations, Costs
In healthcare software engineering since 2005, ScienceSoft implements secure messaging solutions for clinical communication and collaboration (CC&C). Our clients receive tailored messaging systems and workflow extensions that comply with HIPAA/HITECH and internal policies and are based on scalable architectures supporting FHIR and HL7 v2.
Secure Messaging in Healthcare in Brief
Secure messaging in healthcare enables clinicians, administrative staff, and sometimes patients to exchange clinical information (including PHI) safely via encrypted, access-controlled messages rather than unsecured channels such as SMS, personal email, or consumer chat apps.
Poor communication remains a measurable patient safety and liability risk: a 2025 Candello (CRICO) benchmarking report shows that communication-related factors now appear in 40% of asserted US malpractice cases.
Healthcare providers typically go beyond out-of-the-box secure messaging (via custom extensions or a fully custom solution) when:
- Integrations don’t support closed-loop care. OOTB messaging can’t reliably pull context from the EHR and also write outcomes back (e.g., for acknowledgement and escalation), or it can’t ingest critical alerts (lab/radiology, nurse call) into the same trackable workflow.
- Workflows don’t match how sites actually operate. Generic inboxes and routing rules don’t reflect real departmental queues, after-hours coverage, and triage steps, so messages land in the wrong place or create new bottlenecks.
- Governance requirements exceed what the tool can prove. Compliance teams need defensible audit trails, retention and legal-hold options, and enforceable BYOD/MDM policies that many tools can’t satisfy without customization.
- Messaging is fragmented across channels. Clinical team coordination, administrative communication, and (when in scope) patient messaging live in separate tools with different rules, making it hard to enforce consistent routing, escalation, and auditing.
The cost of implementing custom secure messaging in healthcare may range from $80,000 to $800,000+, depending on integration depth (EHR, on-call scheduling, lab, radiology, nurse call, alarms), routing and escalation complexity (roles, queues, rules), security and governance requirements (MDM, BYOD, retention, audit exports), whether patient messaging is included, and other factors. Use our free calculator to estimate the cost of your project.
Core Secure Messaging Functions in Healthcare
- Care team ↔ care team
Clinician-to-clinician messaging for handoffs, consults, and escalation. - Care team ↔ operations/front desk
Clinical-to-operations messaging for routing, intake queues, and scheduling. - Patient ↔ clinic
Patient-to-clinic messaging for non-urgent questions, attachments, guardrails. - Clinical systems → care team (critical results, nurse call/alarms)
System-to-clinician alerts for critical results, nurse calls, and alarms.
It’s important to clearly differentiate secure messaging for regular clinical communication and collaboration (CC&C) from Direct Secure Messaging (DSM). ONC and DirectTrust define DSM as the use of the Direct Standard to exchange health information between healthcare entities (e.g., practices, hospitals, labs) in a trusted network, essentially like secure email across organizations.
ScienceSoft typically delivers DSM as an interoperability layer. We can integrate Direct/HISP capabilities into EHR-centric workflows (addressing/routing, auditing, and documentation), while clinical secure messaging supports day-to-day coordination within your clinic.
Key Capabilities of Secure Messaging Systems for Healthcare
Below are the building blocks, modules, workflows, and capabilities that healthcare providers most often look for in secure messaging solutions. ScienceSoft can implement any combination of them separately or as an extension layer or module on top of your existing secure messaging suite.
Secure conversations
Care teams can communicate in 1:1 and group threads for handoffs, consults, and coordination, with read and delivery status and quick recipient search. Conversations stay synchronized across mobile and desktop, so clinicians can switch between phones and workstations without friction.
Multimodal communication (text, voice, video)
When text isn’t enough, staff can move from secure chat to calling (and, where needed, video) without switching tools. The call stays tied to the same conversation thread, with key details (participants, start/end time, and optional recording links) logged in the conversation. This keeps the full “story” in one place for follow-up, accountability, and auditability across mobile and desktop.
Secure attachments
Clinicians can share clinical photos and documents in a protected thread for faster review and decision-making. Lab/radiology results and other files can be shared as deep links or in-app views from connected systems of record, reducing duplication and the risk of circulating outdated versions. Attachment handling can follow retention and access rules so shared media remains traceable and policy-aligned.
Directories and routing
Clinicians can quickly find the right responsible person by patient, unit, service line, or on-call role, without guessing who is covering the shift or assigned to the patient. Messages can be routed to role-based groups or team inboxes so requests land with the right clinical service from the start.
Urgent messaging escalation
Clinicians can mark a message as urgent and require acknowledgement within a set timeframe. If there’s no response, routing rules automatically escalate the message to the next on-call role or backup responder, creating a traceable escalation chain.
Critical alerting and closed-loop notifications
Clinical systems (e.g., lab and radiology, nurse call, and alarms) can generate notifications that require acknowledgement. The secure messaging system logs who acknowledged and when, tracks escalation if needed, and records closure status back to the source system and the EHR.
Downtime resilience
Secure messaging can be built to remain usable during EHR downtime or network degradation, with defined fallback behavior (e.g., reduced context, manual recipient selection, deferred write-backs). Clinicians can see basic delivery/read indicators in threads, while admins can monitor delivery health via dashboards and alerts to spot delays, failed sends, or degraded connectivity and support safe operations until systems recover.
Adoption controls and alert-fatigue management
Care teams can use message priorities, templates, quiet hours, and routing rules that prevent “broadcast to everyone” patterns. These controls help keep messaging actionable for clinicians and manageable at scale, so teams don’t get swamped by low-priority messages.
Mobile-first security and device controls
Clinicians can work securely on phones and tablets with session timeouts and optional device controls enforced via MDM. Notifications can be configured to prevent PHI from appearing on lock screens, and separate organizational policies can be automatically applied to BYOD vs. managed devices.
Governance and audit trails
Security and compliance staff can review audit trails that show who sent, received, opened, or acknowledged messages, supporting incident investigations and compliance reviews. Governance tools can support access reviews, legal holds, eDiscovery, exportable records, and policies such as no copy/paste or limits on attachment downloads.
Administration and analytics
Admins can configure routing and escalation rules, message types, retention policies, and user roles to align with the organization's realities. Analytics can track messaging volume, acknowledgements, escalations, and response times to help spot bottlenecks and monitor platform performance.
Patient messaging (optional)
Patients can send non-urgent questions and attachments through a secure portal or app inbox that routes requests into role-based queues (front desk, nurse triage, care coordinators). The system can apply guardrails to handle after-hours routing and symptom red flags. Policies then define what gets documented back to the EHR as a link or clinician-approved summary (per policy) to keep the patient record complete and auditable.
How AI Can Support Secure Messaging in Healthcare
AI-assisted triage and routing
AI can classify incoming messages by intent (clinical question, admin request, urgent symptom, critical result) and automatically route them to the right queue or on-call role. Using retrieval-augmented generation (RAG) to draw on provider-specific routing rules, on-call schedules, and triage protocols, an AI agent can suggest priorities and next steps while leaving the final decision to clinicians, contributing to faster response times, fewer missed handoffs, and reduced coordinator workload.
Clinical thread summarization and “handoff-ready” notes
AI can turn long message threads into concise summaries for common clinical workflows such as shift changes, consults, rounding, and similar scenarios. It can also highlight key decisions, pending tasks, and owners with links to specific messages or other sources. Additionally, AI can generate a standardized handoff format (e.g., SBAR or I-PASS) pre-populated with extracted details for clinician review and quick reuse.
Patient messaging copilot with safety guardrails
For patient-facing messaging, AI can draft responses and education snippets grounded via RAG in approved materials (after-visit summaries, FAQs, clinical pathways, medication instructions). The copilot can detect potential red-flag symptoms and, based on predefined guardrails, trigger appropriate actions (e.g., prompting the patient to seek emergency care or rerouting messages after hours) before human review, enabling faster responses and more consistent guidance.
Important Integrations for a Secure Messaging System in Healthcare
To enable smooth and secure messaging between care teams, integrations are key. Below, ScienceSoft’s architects show the most likely integration pathways for clinical secure messaging tools.
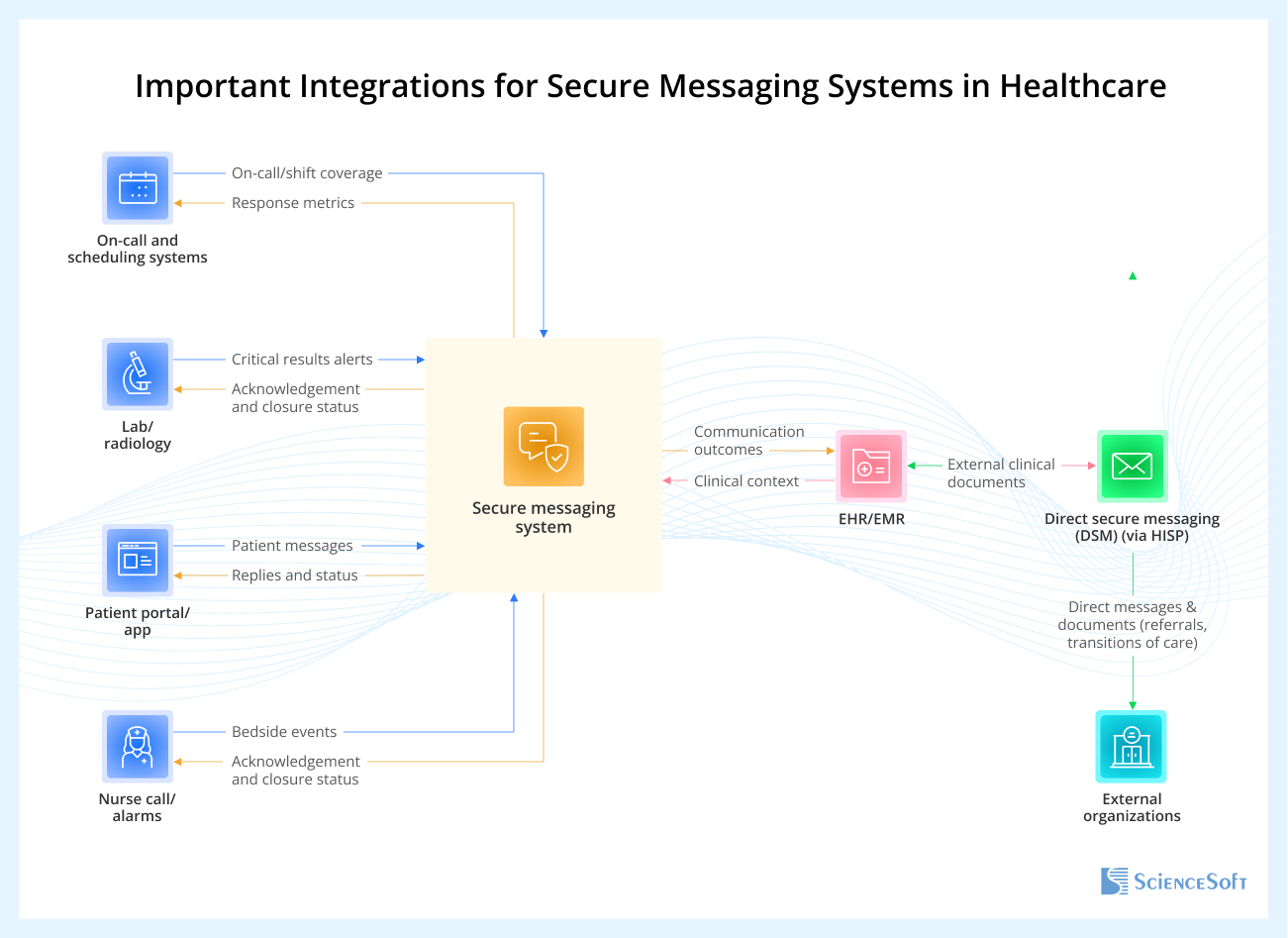
- An EHR/EMR integration provides patient and encounter context and can link messages to orders or results. Key communication outcomes (e.g., acknowledgements, escalation status, and a link back to the secure messaging thread or an approved summary of the conversation and decisions) can be recorded back to the EHR. When cross-organization exchange is needed, Direct Secure Messaging (via a HISP) can be integrated into EHR workflows for referrals and transitions of care.
- Integration with scheduling or on-call systems ensures messages go to the right person at the right time. It uses shift rosters, on-call assignments, and coverage rules to route urgent messages correctly and apply escalation paths if there is no response.
- A patient portal or patient app integration enables secure, asynchronous patient messaging without using consumer chat apps. Patient requests can be routed to the right queue based on the message topic/type, selected department or care program, the patient’s care team, location, or scheduling/triage rules. Patients can read care team responses in the portal/app, see message status (e.g., delivered/read), and receive privacy-safe notifications that don’t include PHI and prompt them to open the portal/app for details.
- Integration with laboratory and radiology systems enables sending critical results alerts with patient context and priority through secure messaging, so the right clinician is notified quickly. Acknowledgement and closure status can be sent back to support closed-loop follow-ups.
- Integration with nurse call, alarm management, and remote patient monitoring systems brings bedside events into secure messaging with patient context (including location/room) and urgency indicators. Acknowledgement, escalation, and closure status can be returned to prove alerts were received and resolved.
Implementation and Development of Secure Messaging in Healthcare: Best Practices
ScienceSoft experts share field-tested practices to make secure messaging reliable in real clinical workflows with fast routing to the right on-call clinician, fewer missed handoffs, and defensible audit trails.
Design for downtime and degraded conditions from day one
EHR and on-call integrations are common points of failure: when they’re slow or unavailable, secure messaging can lose patient context or route to the wrong responder. Best practice is to support a degraded mode (manual recipient selection, cached coverage with timestamps) and make EHR write-backs asynchronous with retries and clear “pending documentation” statuses. For critical workflows, escalation should route to a staffed team inbox (e.g., charge nurse desk, unit coordinator, or centralized triage/operations center) when on-call data is unavailable, so a human can assign the request to the right clinician instead of the system auto-picking a “best guess” based on stale coverage.
Add a custom workflow layer to existing secure messaging with low-code tools
Out-of-the-box secure messaging often lacks the tools to set up custom message intake and routing workflows, so requests end up in personal inboxes and teams resort to broadcasting messages to “whoever might answer.” But that doesn’t mean you need to rip and replace your existing CC&C platform. Many providers keep their existing messaging and add a workflow layer with low-code apps (e.g., Microsoft Power Apps) for intake queues, triage screens, routing dashboards, templates, and admin controls (ownership, after-hours rules, escalation timers). Low-code modules are generally cheaper and faster to deliver than fully custom-coded software components. Plus, healthcare-aware vendors like Microsoft provide enterprise security and compliance controls for their low-code platforms that can support HIPAA requirements.
Standardize governance and audit controls across messaging tools and BYOD environments
Secure messaging governance breaks when policies differ by tool (e.g., one retains messages for 30 days, another for 7 years), and audits become manual screenshot hunts. A stronger approach is to define a single policy baseline (roles, who-can-message-whom, retention by message type, export format, escalation evidence) and centralize logs and exports into a consistent audit trail. If BYOD is allowed, enforce app-level controls (PHI-safe notifications, session timeouts, attachment restrictions) and use MDM selectively for higher-risk roles (device encryption, screen lock, selective wipe), so compliance doesn’t depend on personal phone settings.
Migrate from pagers workflow-by-workflow and prove acknowledgements
Attempts to retire pagers and adopt secure messaging stall when staff keep using both channels (page and chat) for the same workflow, and there is no reliable way to track acknowledgement and escalation for time-critical requests. Avoid a big-bang switch: migrate workflow-by-workflow, starting with flows that require acknowledgement (e.g., critical results), then on-call escalation, then routine unit coordination, while mapping pager groups to role-based recipients. Run a short, time-boxed parallel period (using paging only as a fallback, not an alternative channel) for each workflow and track acknowledgement time, missed acknowledgements, and escalation rates. Retire paging for that workflow once targets are met, then move to the next.
Costs and Cost Drivers for Secure Messaging Systems in Healthcare
The cost of implementing secure messaging in healthcare typically ranges from $80,000 to $800,000+.
The biggest cost drivers are:
- Number of integrations (EHR or EMR, on-call scheduling, lab, radiology, nurse call software, etc.).
- Existing CC&C tool stack and the capacity for its evolution (e.g., to migrate data, change platforms, extend, or add a workflow layer).
- Number of user groups and routing rules (how many departments or roles need different inboxes, priorities, escalations, and after-hours workflows).
- Mobile security model (BYOD vs. corporate devices).
- Audit and retention requirements (how detailed activity logs must be and for how long messages and attachments must be stored).
- Device strategy (how many device types must be supported and managed: iOS/Android, tablets, shared devices, MDM-managed vs. unmanaged).
Based on ScienceSoft’s project experience, the typical implementation cost ranges are the following. Note that licensing or subscription costs (for EHR or messaging platforms) are not included.
$80,000–$150,000+
To select and implement a market-available secure messaging platform, integrating it with your clinical stack (e.g., EHR, SSO, and scheduling) and configuring core workflows for message intake and routing.
$80,000–$150,000+
To add a workflow layer on top of your existing secure messaging platform or EHR messaging with triage queues, routing dashboards, templates, audit exports, and lightweight automation (using low-code first development).
$150,000–$300,000+
To develop custom modules or components for your out-of-the-box messaging platform, such as complex routing and escalation logic, specialized integrations, or constrained BYOD or MDM security requirements.
$300,000–$800,000+
To engineer and roll out a highly customized enterprise-scale solution. It may cover CC&C across multiple facilities, custom data retention logic, SIEM and MDM alignment with internal policies, deep EHR and clinical-event integrations, patient messaging at scale, and assistive AI features.
Want a more precise figure?
ScienceSoft’s team is ready to provide a quote for your specific case.
Why ScienceSoft
- In healthcare IT since 2005.
- Principal architects with experience in implementing enterprise-scale integrations and secure data exchange.
- Experience in achieving compliance with HIPAA/HITECH, GDPR, PDPL, and 42 CFR Part 2.
- Deep knowledge of interoperability standards such as FHIR and HL7 v2.
- Expertise in healthcare security and identity management: SSO, MFA, RBAC, audit trails, encryption, and MDM-enabled device controls.
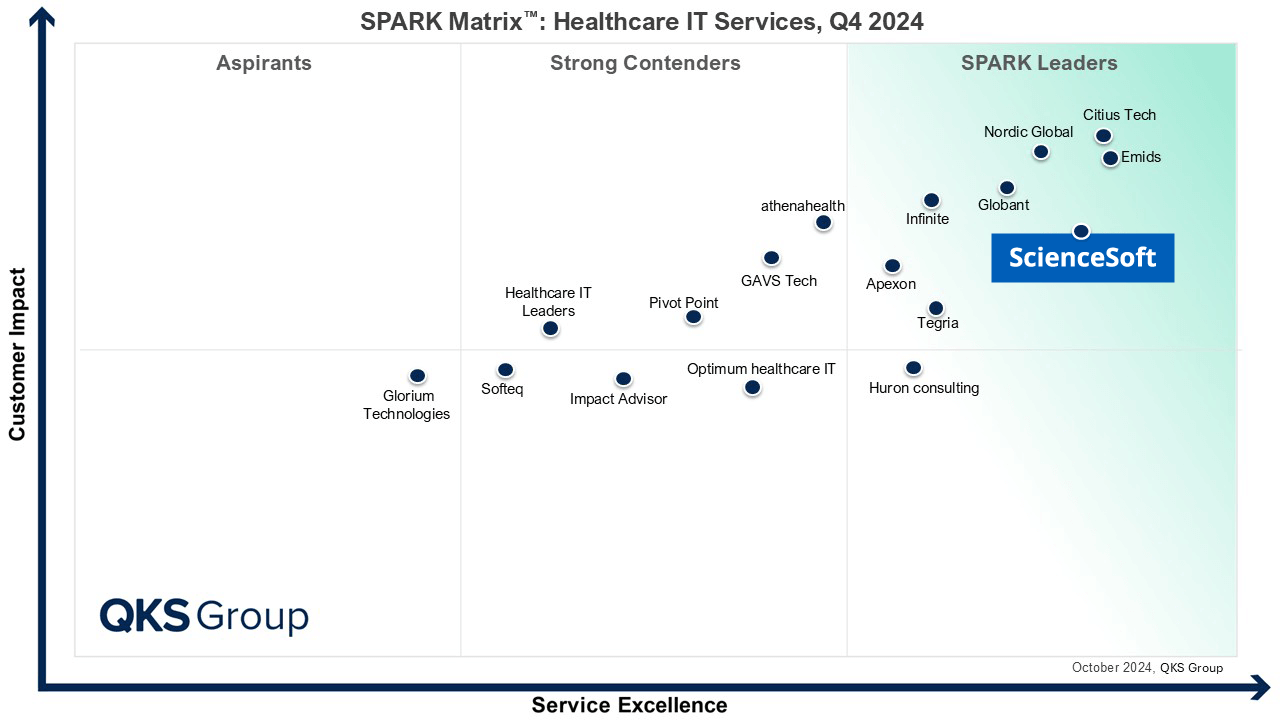
Featured among Healthcare IT Services Leaders in the 2022 and 2024 SPARK Matrix
Recognized for Healthcare Technology Leadership by Frost & Sullivan in 2023 and 2025
Named among America’s Fastest-Growing Companies by Financial Times, 5 years in a row

Top Healthcare IT Developer and Advisor by Black Book™ survey 2023
Four-time finalist across HTN Awards programs

Named to The Healthcare Technology Report’s Top 25 Healthcare Software Companies of 2025

HIMSS Gold member advancing digital healthcare
ISO 13485-certified quality management system
ISO 27001-certified security management system




