EHR for Obstetrics and Gynecology (OB/GYN)
Capabilities, Integrations, and Development Costs
In healthcare IT since 2005, ScienceSoft delivers full-scale EHR solutions and focused OB/GYN extensions that give providers stronger care continuity, cleaner data exchange, tighter disclosure control, and fewer losses tied to fragmented billing workflows.
EHR for Obstetrics and Gynecology in Brief
An obstetrics and gynecology EHR provides a shared clinical record for prenatal care, gynecology visits, labor documentation, postpartum follow-up, and newborn-related handoffs. OB/GYN EHR modules for ambulatory practices and women’s health clinics can also support prenatal episode tracking, visit documentation, preventive follow-up, and patient communication. Hospitals and perinatal service lines often need added support for labor and delivery operations, mother-baby record linkage, fetal monitoring, and postpartum transitions. Health systems and multi-site providers may also need a shared women’s health layer for consistent data exchange, reporting, and disclosure controls across locations.
A custom obstetrics and gynecology EHR system is most justified when ready-made EHR or OB/GYN platforms leave gaps in specialty operations. Typical pressure points are prenatal and inpatient continuity, partner-specific data exchange, reproductive-health disclosures, maternity billing, reporting, and bedside data flows. Ambulatory women’s health practices and perinatal care providers typically choose the following custom solution paths:
- Focused OB/GYN extensions when providers want to keep the current EHR and add prenatal episode management, specialty documentation, preventive follow-up, or procedure workflows in one governed layer.
- A patient engagement layer when providers need to unify portal tasks, intake, scheduling, education, and remote updates in one patient journey connected to the EHR.
- An interoperability and reporting layer when providers need to centralize partner exchange, hospital handoffs, payer workflows, quality reporting, and disclosure controls without redesigning the core EHR.
- A full-scale OB/GYN clinical platform when providers need one coordinated environment for ambulatory, inpatient, and postpartum workflows, reporting, and partner exchange while the enterprise EHR remains the certified core.
|
|
|
|
|
Useful integrations for an EHR for OB/GYN: scheduling systems, patient portals, LIS, RIS, PACS, pharmacy systems, RPM tools, perinatal monitoring systems, HIEs, payer systems, and quality reporting registries. Implementation time: 6–10 months for a focused extension or specialty module, and 12–20+ months for a multi-module solution. Development costs: from $120,000 for a narrow operational layer to over $2,200,000 for enterprise obstetrics and gynecology software with device integrations, advanced reporting, and optional AI modules. Use our free calculator to get a case-specific estimate. |
|
|
|
Main Capabilities of OB/GYN EHR Software
Below are the main OB/GYN EHR features most often requested by ambulatory women’s clinics, hospitals, and health systems with perinatal service lines. ScienceSoft can deliver any selection of these capabilities as narrow functional modules or full-scale OB/GYN solutions, depending on each provider’s needs and existing IT tool stack.
Ambulatory OB/GYN clinical workflows
Inpatient perinatal care operations
Clinician productivity and revenue integrity
Patient experience and remote care
High-Impact AI Modules for OB/GYN EHR Workflows
ScienceSoft helps women’s health providers build HIPAA-aligned AI modules for OB/GYN EHR environments to free up clinician time, expand appointment capacity, and support consistent documentation quality across clinics, service lines, and locations.
Each use case described below can start as a narrowly scoped component, with clear data boundaries, auditability, and mandatory human review, and then scale when results and governance meet leadership expectations.
AI scribe for OB/GYN documentation
Such tools can produce EHR-ready draft notes from clinician-patient conversations during prenatal visits, postpartum follow-ups, gynecology consultations, and procedures. They can also structure text into configured note sections, flag missing history details, support coding, and prepare a review-ready summary.
Reported benefits: ~20% less time in notes per appointment and ~13 percentage-point drop in staff burnout rate with AI scribing.
AI for patient access and self-service
Such tools can answer routine prenatal and gynecology questions in the patient portal, support self-scheduling for suitable visit types, provide visit-ready instructions, and collect structured request details. They can hand low-certainty or high-risk conversations to staff, draft follow-up replies, and route messages to the right work queues.
Expected benefits: shorter response times for routine requests, more consistent portal communication, and lower staff workload.
AI-assisted prior authorization and claiming
Such tools can extract diagnoses, procedures, medications, and prior treatment history from the record, compare them with payer rules, suggest codes and modifiers, and flag missing support before submission. They can also draft prior authorization requests, denial appeal letters, and coder review tasks from the supporting record.
Reported benefits: ~25–50% reduction in coding-related denials with AI coding.
AI-assisted pregnancy risk flagging and pathway orchestration
An NLP module can extract documented risk factors from both structured and unstructured EHR data, identify patients who may need closer review, and support clinician-led risk stratification for prenatal outreach, monitoring, and care-pathway assignment.
Reported benefits: up to 2x higher capture of at-risk patients with NLP-based EHR screening.
Important Integrations for OB/GYN EHR
In OB/GYN electronic health record projects, integrations often decide whether clinical teams will see outside records in time, whether payers will respond before scheduling, and whether quality submissions will reflect reality.
The integration architecture design starts with what must stay consistent across systems: patient identity, encounter context, and mother-newborn linkage, so orders, results, and safety checks land in the right chart. Then, ScienceSoft’s solution architects choose partner-ready data exchange formats: FHIR or HL7 for clinical exchange, X12 or FHIR for payer transactions, NCPDP for ePrescribing, and QRDA formats for CMS eCQM submissions. Typically, they also establish end-to-end data flow tracking with message queues, retries, and an exception worklist that assigns owners, timestamps, and next actions. This way, message delays can be caught before they affect care or billing.
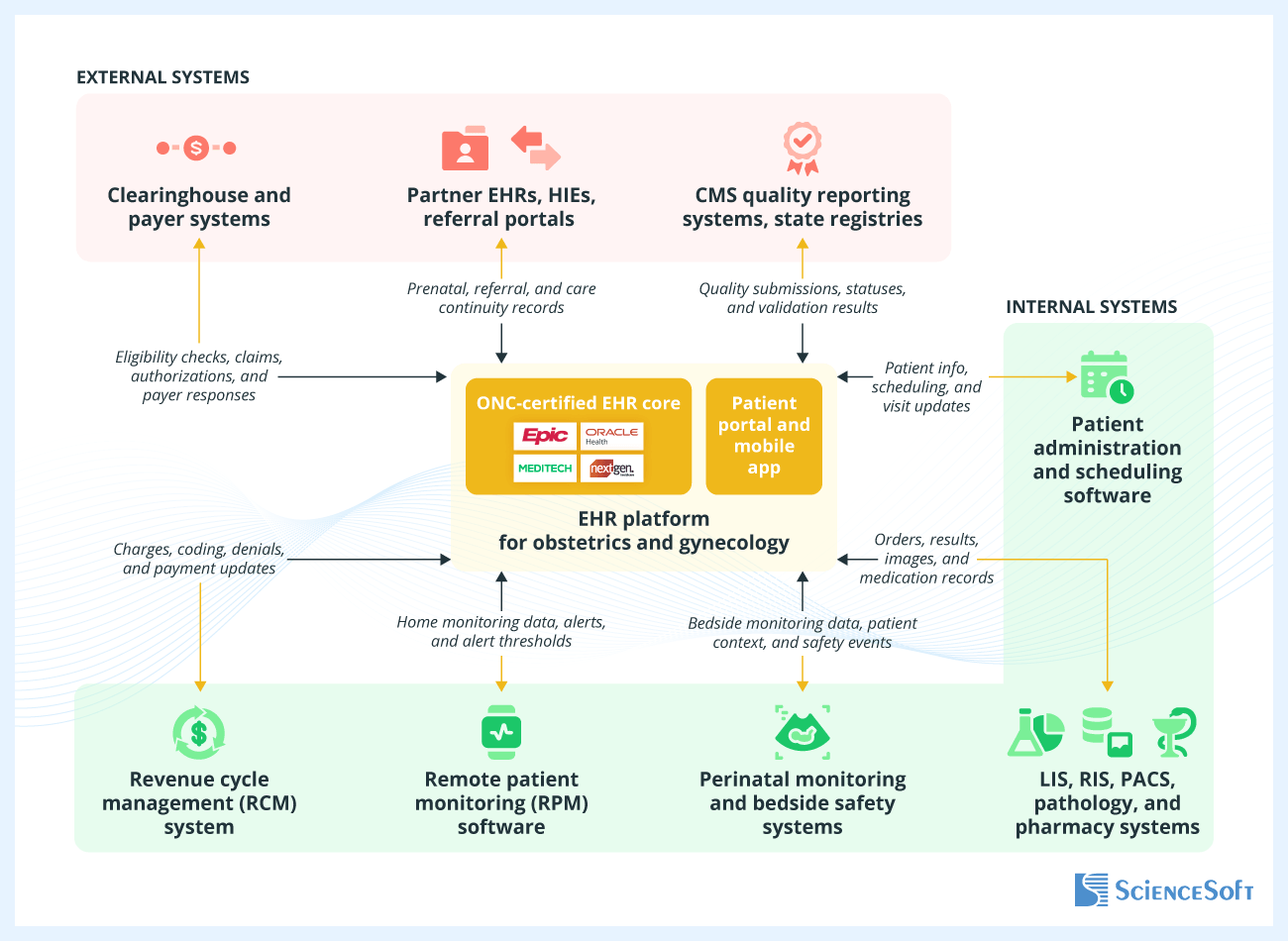
- Patient administration and scheduling software — to keep identity and appointments consistent for prenatal care and gynecology visits; to prevent duplicate charts and mismatches during transfers and specimen collection.
- LIS, RIS, PACS, pathology, and pharmacy systems — to trigger prenatal and gynecology workflows from visit notes; to surface imaging, pathology, and medication updates in views and follow-up worklists.
- Revenue cycle management (RCM) software — to align gynecology procedures and prenatal encounters with coding rules; to apply maternity package logic across episodes and reconcile charges before billing cutoffs.
- Remote patient monitoring (RPM) software — to collect patient-submitted vitals in triage queues for nurse review; to adjust monitoring protocols by risk group without manual data re-entry.
- Perinatal monitoring and bedside safety systems — to link fetal monitoring and feeding safety devices to the patient chart; to enable escalation review and verification during labor and postpartum care.
- Partner EHRs, HIEs, referral portals — to review outside obstetric and gynecology history during admissions and consults; to deliver structured handoffs that shorten intake and support specialist follow-through.
- CMS quality reporting systems, state registries — to submit evidence for maternity outcomes and gynecology screening measures; to validate quality KPIs with feedback so teams correct data gaps before submission.
- A clearinghouse and payer systems — to confirm benefits for pregnancy care and gynecology procedures before scheduling; to route payer rejections into coder worklists so teams can correct supporting documentation earlier.
Other frequently requested integrations include:
- Identity and access management services — to unify clinician sign-in across clinical apps and portals and enforce least-privilege access and audit logs for HIPAA reviews.
- Document intake and consent tools — to ingest outside records into pregnancy episodes without manual indexing; to capture e-signatures for procedures and releases in clinic workflows.
- Payment gateway and patient billing tools — to collect copays and balances during digital check-in; to post payment status into finance workflows without manual reconciliation.
- Enterprise analytics and data warehouse tools — to consolidate maternal quality and gynecology performance metrics across sites; to support tuning for CDS and follow-up worklists based on outcomes.
Development Tips for OB/GYN EHR Projects
Below, ScienceSoft’s experts highlight three engineering decisions that reduce hidden delivery risks and keep the software predictable for clinical, operational, and IT teams.
Pregnancy episode and mother-baby dyad as a first-class data model
Pregnancy documentation often gets split across visits, while the newborn record lives in a separate chart. IT teams typically try to fix it by adding one-off mapping rules and workarounds, and then revisiting them when upstream fields change. The hidden cost is interface rework and clinical time lost to resolving mismatches between maternal and newborn data.
ScienceSoft recommends building a data model in which the pregnancy episode and the mother-baby dyad are core records, with shared identifiers and time-ordered events. This foundation supports maternity analytics, interoperability, and a clear source of truth across prenatal, labor, delivery, and postpartum care.
Reproductive-health privacy by design
OB/GYN providers often face high-risk record requests that involve reproductive-health data. As disclosure rules and request types change, they often exceed what EHR release workflows can document and prove in an audit. Then, staff try to collect attestations and approvals in emails or shared files and manually override disclosure rules, but this creates audit gaps, rework, delays, and legal exposure.
ScienceSoft’s architects recommend building an EHR-embedded disclosure service with a rules engine that keeps privacy policies as versioned, effective-dated decision sets. When disclosure rules change, teams can update the active decision set without rewriting application code or reworking the release workflow. In a centralized change workflow, OB/GYN compliance staff can draft updates, the legal team can approve them, and the provider’s IT team can publish a new policy version and link it to each disclosure record. This approach shortens sensitive-request turnaround, produces defensible audit trails, and reduces regression defects when policies change.
RAG-grounded content governance for OB/GYN policy search and patient education
OB/GYN teams often keep triage guidance, postpartum warning-sign instructions, and patient education content in separate documents, portal pages, and internal knowledge repositories. Staff then search several sources, reuse old message templates, or rely on generic AI assistants when preparing patient portal replies or internal answers. That can result in inconsistent or outdated guidance and also creates safety and privacy risks.
ScienceSoft recommends organizing this content as a governed knowledge base that supports policy-aware retrieval through regular enterprise search and also powers retrieval-augmented generation (RAG) through a controlled LLM assistant. In the assistant flow, retrieval keeps answers tied to approved, versioned OB/GYN protocols and patient education materials, tagged by audience, effective date, and care stage. Staff can use this setup for policy lookup and drafting education content. Our engineers ensure that the architecture separates staff and patient materials, keeps protected health information out by default, and sends symptom-based or low-confidence patient messages to clinical staff.
How Much It Costs to Develop an OB/GYN EHR Solution
Development costs for an obstetrics and gynecology EHR extension or clinical platform vary from $120,000 to over $2,200,000. The main cost drivers are the range of care processes covered, the number of connected systems, the need to process live data from bedside devices, and the addition of advanced reporting or AI-assisted functions.
The ranges below exclude third-party vendor fees, infrastructure and hosting costs, transaction fees for connected services, and long-term support.
$120,000–$180,000
A low-code OB/GYN workflow extension covering one narrow operational layer around the current EHR. For example, it can include digital intake, consent routing, staff worklists, and one or two basic data exchanges.
$250,000–$550,000
An OB/GYN module for an existing EHR covering one specialty workflow set. For example, it can include prenatal episode management, visit templates, results follow-up, and a small group of supporting interfaces.
$600,000–$1,200,000
A multi-module OB/GYN extension combining two or three connected workflows around the current EHR. Typical scope joins specialty workflows, patient portal functions, reporting, and several system interfaces under shared business rules.
$1,200,000–$2,200,000+
A custom women’s health platform designed to extend existing clinical systems across outpatient and inpatient workflows. Depending on the case, it may support ambulatory care, labor and delivery, mother-baby linkage, device connectivity, reporting, multi-site interoperability, and AI features.
Low-code platforms such as Power Apps can reduce development time and cost because they let you assemble workflow apps from prebuilt components instead of coding every layer from scratch. In my experience, this works best for OB/GYN providers who want to keep their current EHR and add a few specialty workflows fast, for example, intake checks, consent routing, prenatal follow-up queues, or quality-data correction worklists.
It stops being a good fit when those apps start carrying complex integrations, strict access rules, audit-sensitive logic, or core care workflows that need to stay consistent across systems and over time. That is why a hybrid setup is often the safer option: low-code for internal admin and coordination workflows, custom code for functions such as mother-baby linkage, bedside data flows, patient-facing journeys, and more demanding AI features.
Why Choose ScienceSoft for Your OB/GYN EHR Project
- Since 2005 in healthcare software engineering with 150+ successful projects, including EHR modernization, extension, and integration.
- 750+ IT specialists, including in-house MD consultants and solution engineers with healthcare backgrounds.
- 20+ principal architects with 15–25+ years of experience to keep OB/GYN EHR architectures scalable, auditable, and maintainable.
- Hands-on experience with meeting HIPAA, HITECH, ONC, and the 21st Century Cures Act requirements.
- EHR integration expertise across HL7 v2/v3, FHIR, USCDI, CCDA, and XDS/XDS-I, with clinical terminology mapping for SNOMED CT, LOINC, RxNorm, ICD-10-CM/PCS, CPT/HCPCS, and more.
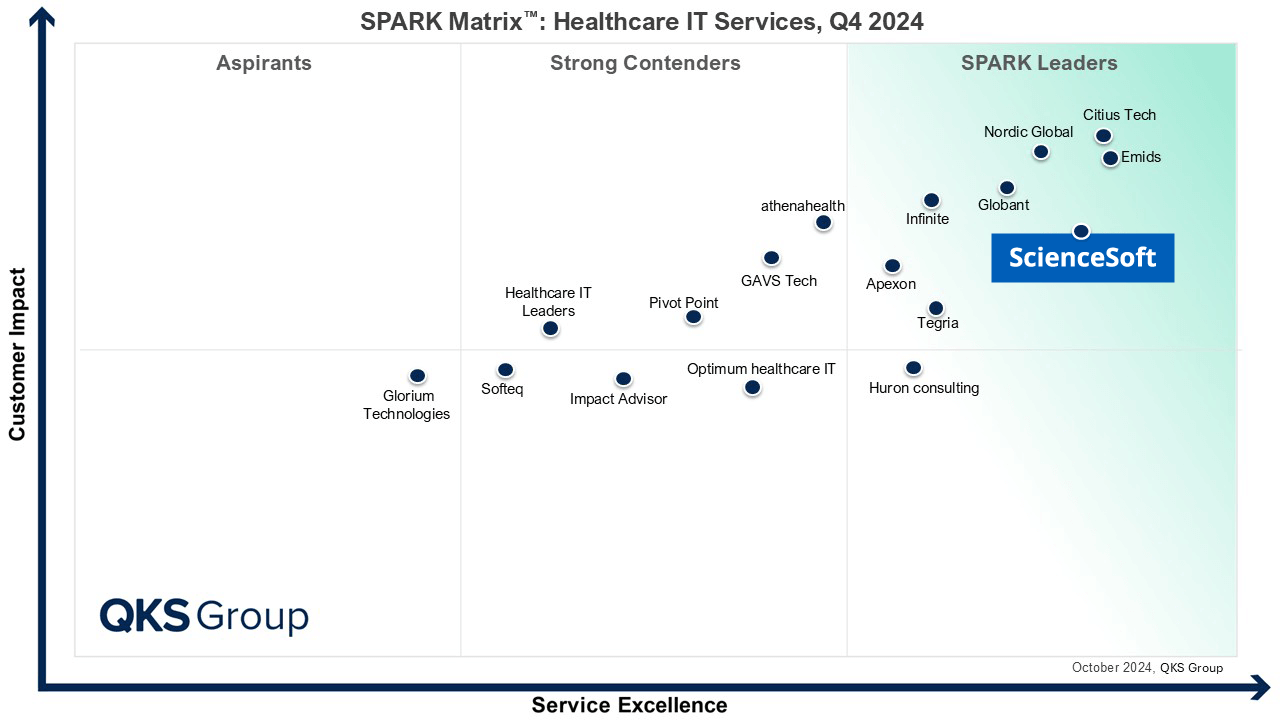
Featured among Healthcare IT Services Leaders in the 2022 and 2024 SPARK Matrix
Recognized for Healthcare Technology Leadership by Frost & Sullivan in 2023 and 2025
Named among America’s Fastest-Growing Companies by Financial Times, 5 years in a row

Top Healthcare IT Developer and Advisor by Black Book™ survey 2023
Four-time finalist across HTN Awards programs

Named to The Healthcare Technology Report’s Top 25 Healthcare Software Companies of 2025

HIMSS Gold member advancing digital healthcare
ISO 13485-certified quality management system
ISO 27001-certified security management system




