Telemedicine Apps for Rural Areas
Features, Architecture, Costs
In healthcare IT since 2005, ScienceSoft designs and implements reliable telemedicine software for care delivery in rural areas.
Telemedicine in Rural Areas: the Essence
Telehealth enables virtual healthcare services for rural residents, improves patient self-monitoring, reduces avoidable trips for patients and medical staff, and decreases the risk of complications. In the US, rural areas comprise about two-thirds of the primary care health professional shortage areas, spurring the increase in demand for rural telehealth services.
Custom telehealth software is vital for rural resident care as it can be specifically tailored to address unique backcountry challenges. These may include limited connectivity in remote areas, compatibility with localized healthcare systems, integration with regional health data repositories, and adherence to specific rural healthcare policies or regulations.
Based on ScienceSoft’s experience, developing a custom telehealth platform for rural areas may cost from $150,000 to $400,000 and depends on the system's complexity (e.g., advanced features or legacy software integrations). Use our free cost calculator to estimate the cost for your case.
The Architecture of Telemedicine Software for Rural Areas
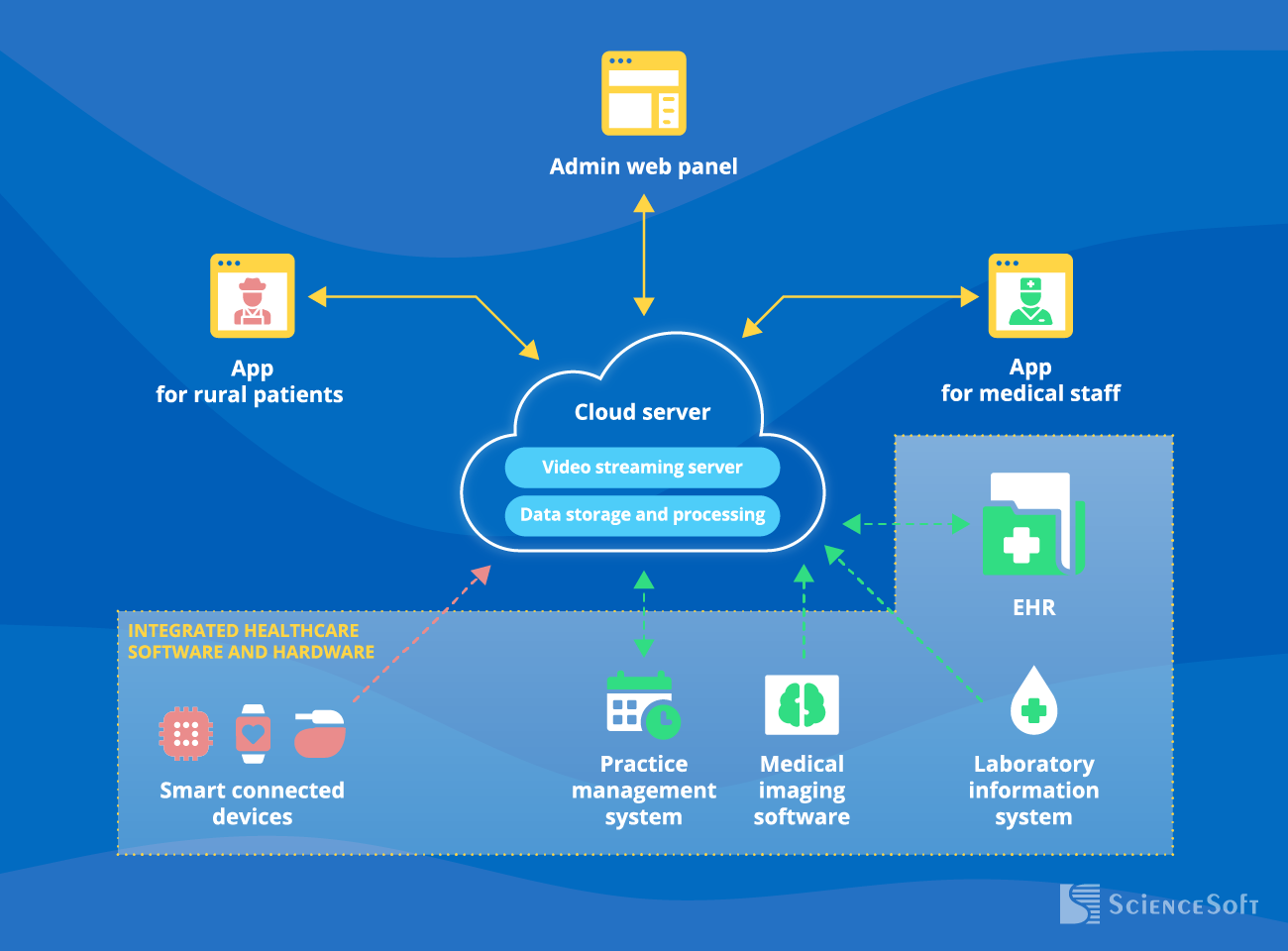
At the core of the telemedicine solution for rural areas is a cloud server with a video streaming server and a data storage and processing module. The former enables real-time audiovisual communication between medical staff and patients. The latter stores patient-doctor video appointments history and recordings, messaging history, shared images (e.g., photos of wounds), PHI (e.g., logged symptoms and vitals), and more.
Other vital modules of rural telehealth software include:
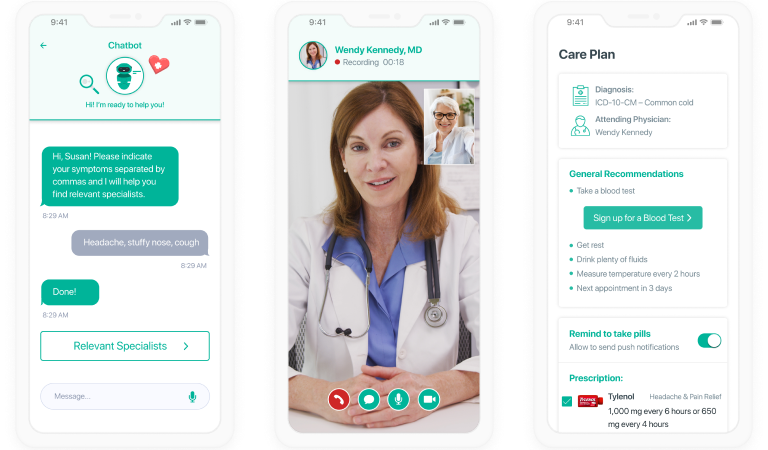
App for rural patients
- To schedule and visit online consultations with medical staff (a physician, a nurse, etc.).
- To consult a doctor on disease symptoms (e.g., cough) via messaging.
- To log vitals and symptoms in the app.
- To access and use educational materials on self-monitoring, home care, and rehabilitation.
Show more
App for medical staff (physicians, nurses, etc.)
- To conduct online appointments and regular health checkups for rural patients.
- To manage patient treatment and medication plans.
- To schedule remote consultations with other specialists for rural patients.
- To monitor patients’ health state.
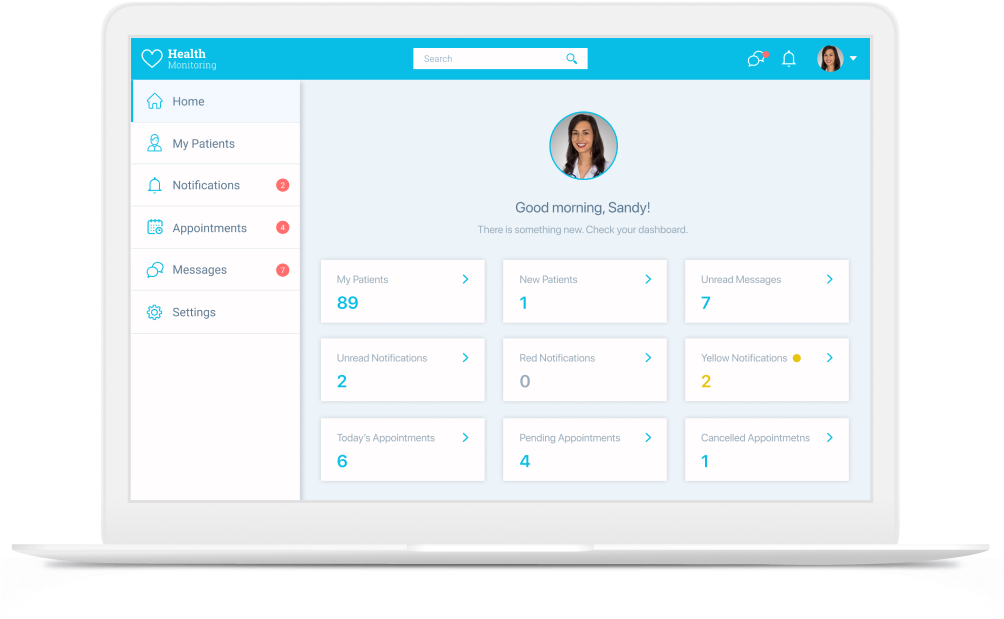
Admin web panel
For hospital supervisors, telehealth program administrators, etc., to:
- Process emergency care requests from rural residents.
- Edit the list of rural telehealth app users (e.g., add users from new service regions).
- Manage access rights of rural telehealth app users.
- Manage medical staff’s schedules, etc.
Key Features of Rural Telemedicine Software
Based on its experience in healthcare IT since 2005, ScienceSoft describes common and advanced functionality of a telehealth system for rural patients.
How to choose features for a rural telemedicine app?
When deciding on the telehealth application functionality, I recommend starting with a thorough analysis of target users. For example, suppose many of your patients have chronic diseases and require continuous tracking of health parameters. In that case, it may be feasible to add remote patient monitoring functionality and integrate the app with wearables or smart medical devices.
Important Integrations for a Telehealth App for Rural Areas
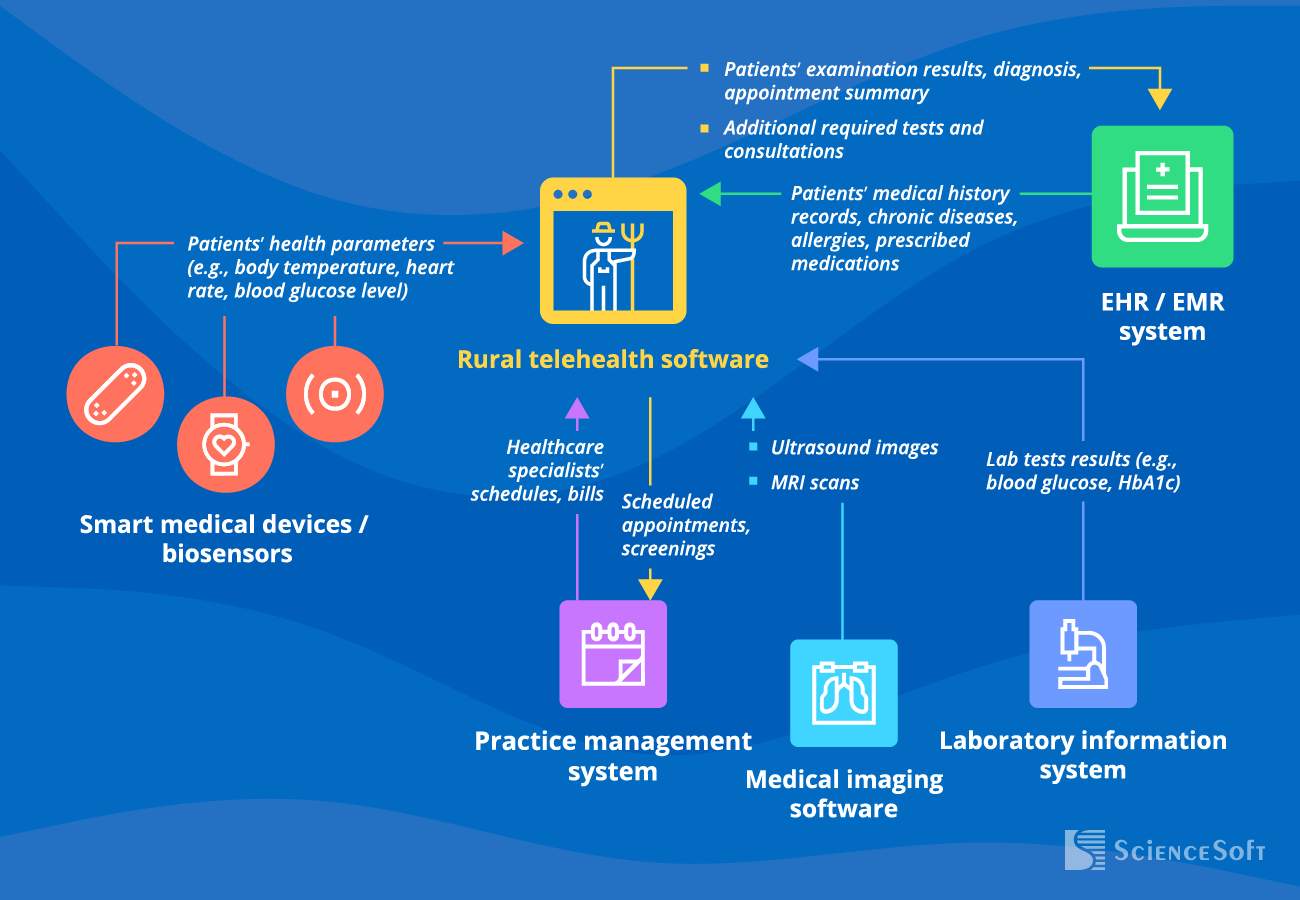
ScienceSoft's healthcare IT consultants find it important to integrate telemedicine software with the following systems to achieve patient data exchange automation:
- For an integrated view of rural patients’ medical history (chronic conditions, allergies, etc.).
- For automated visit logging in EHR and streamlined billing.
- For EHR-enabled integrations with accounting software, e-prescribing software used by pharmacies in the service region, etc.
Smart medical devices or biosensors
- To enable collection and processing of rural patients’ vitals (e.g., blood pressure, body temperature).
- To enable in-app monitoring of rural patients’ vitals by medical staff.
Medical imaging and lab software
- To enable in-app access to patients’ medical images.
- To provide doctors and patients with direct access to test results (HbA1c level, blood glucose, etc.) issued by any partnering local laboratory.
- To enable in-app access to medical specialists’ schedules for an administrator, a doctor, or a patient.
- For automated medical services billing, accounting, etc.
How to Develop Telehealth Software for Rural Areas
To deliver custom telemedicine software for rural residents, ScienceSoft follows the key development steps outlined below:
1
Identification of essential features, such as remote patient monitoring, audio/video consultations, and patient record management, to ensure seamless healthcare delivery in rural settings.
2
Definition of a resilient and adaptable software architecture and tech stack design for optimized performance in low-bandwidth internet environments.
3
Detailed planning to establish project goals, timelines, and allocate resources.
4
Incremental development of an accessible and responsive telehealth software solution.
5
Implementation of necessary security measures to safeguard patient information.
6
Rigorous testing of the software across different network conditions to ensure its high performance.
7
Integration with a wide range of connected medical devices for home use (e.g., wrist and finger pulse oximeters, remote health examination kits, portable ECG monitors, handheld ultrasound scanners), enabling rural residents to perform diagnostic tests under remote supervision.
8
Smooth software deployment, taking into account the specific infrastructure limitations of rural areas, such as unreliable internet connectivity and power supply.
9
Ongoing support and maintenance to ensure the software remains up-to-date, continues to meet the evolving needs of all user groups, has no bugs, and boasts the most advanced features.
What Determines the Success of Telehealth for Rural Areas
|
|
Communication stabilityTo tackle remote communication issues in rural regions, your app needs to provide various connection modes (e.g., switching to audio-only using VoIP or cellular network message-based communication in case of poor internet connection). Adding fallback options and automatic video quality adjustment ensures that both patients and medical specialists can stay connected without interruptions to care. |
|
|
Smooth integration with healthcare IT systemsTo provide medical specialists with up-to-date patient data and help them remotely deliver care to rural patients, you should ensure timely access to all needed information from integrated EHR, LIS, medical imaging software, etc. Using widely adopted standards such as FHIR, USCDI, and CCDA helps simplify integration across different systems, while employing clinical terminologies like SNOMED CT, LOINC, and RxNorm keeps clinical data consistent throughout the ecosystem. |
|
|
Intuitive, user-friendly UX/UITo ensure that rural patients of any age and tech proficiency can comfortably use the app, focus on the usability and accessibility of telehealth software from the very start. Clear navigation, simple workflows, and accessibility features (e.g., larger fonts, voice guidance) make the platform inclusive and reduce barriers for first-time users. |
Investments and ROI

The development of a rural telemedicine app may cost from $150,000 to $400,000. Core communication and care planning features are covered at the lower cost, while advanced functionalities like patient data analytics and RPM account for the higher price.
Depending on the number of telehealth visits, the number of medical staff members, and other service factors, a rural telehealth solution can reach 100% ROI in ~6 months.
Want to know the costs of your rural telehealth software?
Learn more about telemedicine software development cost factors and ROI.
Key financial benefits
|
|
Expanded service area due to the ability to deliver care to hard-to-reach population groups, underserved regions, etc. |
|
|
Decreased length of postoperative hospital stay for rural patients and lowered readmission rate by 31% due to telehealth-supported home care and rehabilitation. |
|
|
Mitigated medical staff shortage in the service regions due to improved medical specialists’ efficiency, optimized schedules, and decreased travel time. |
|
|
Reduced operational expenses per rural patient (including efficient bed allocation) for hospitals due to decreased hospitalizations of about 70% of remotely monitored patients with chronic diseases and other conditions. |
|
|
Improved visit attendance (for patients with chronic conditions, mental health conditions, etc.). |
Examples of Telemedicine for Rural Areas

Horizon Health Alliance, a mental healthcare provider based in Buffalo, New York, implemented a telehealth solution and now serves 70% of patients virtually. Within a year, Horizon has served 891 unique patients from rural areas with limited access to mental health and substance use disorder services.
SA Health, Australia, implemented a telehealth platform for rural residents to gather vital health information from stroke patients and provide virtual consultations. As a result, it doubled its rural treatment capacity and reduced unnecessary hospital-to-hospital transfers by 72%.

Riverwood Healthcare Center in Aitkin, Minnesota, quickly deployed a telehealth solution for the virtual treatment of patients during the coronavirus pandemic. Now, the center has rolled out the new model of care to its family physicians, specialty providers, and rehabilitation therapists.
Why Opt for Custom Telehealth Software for Care Delivery to Rural Areas
ScienceSoft's healthcare IT consultants recommend that you choose custom development of a telehealth app for rural patients if you need:
Functionality tailored to the needs of a healthcare organization and rural patients
Software covers a wide array or a specific set of healthcare services and precisely fits into the healthcare organization’s workflows. For one of our clients, we combined a telehealth solution with a practice management system to ensure convenience for medical staff.
Advanced data analytics
Analytics of patient symptoms and vitals to predict the course of the disease, potential complications, and risks, optimize the set of required telehealth services for rural patients.
Telehealth Software for Rural Areas by ScienceSoft
With 150+ successful healthcare IT projects in our portfolio, ScienceSoft has extensive practical experience in telemedicine and is ready to design and implement telehealth software tailored to the needs of rural residents.
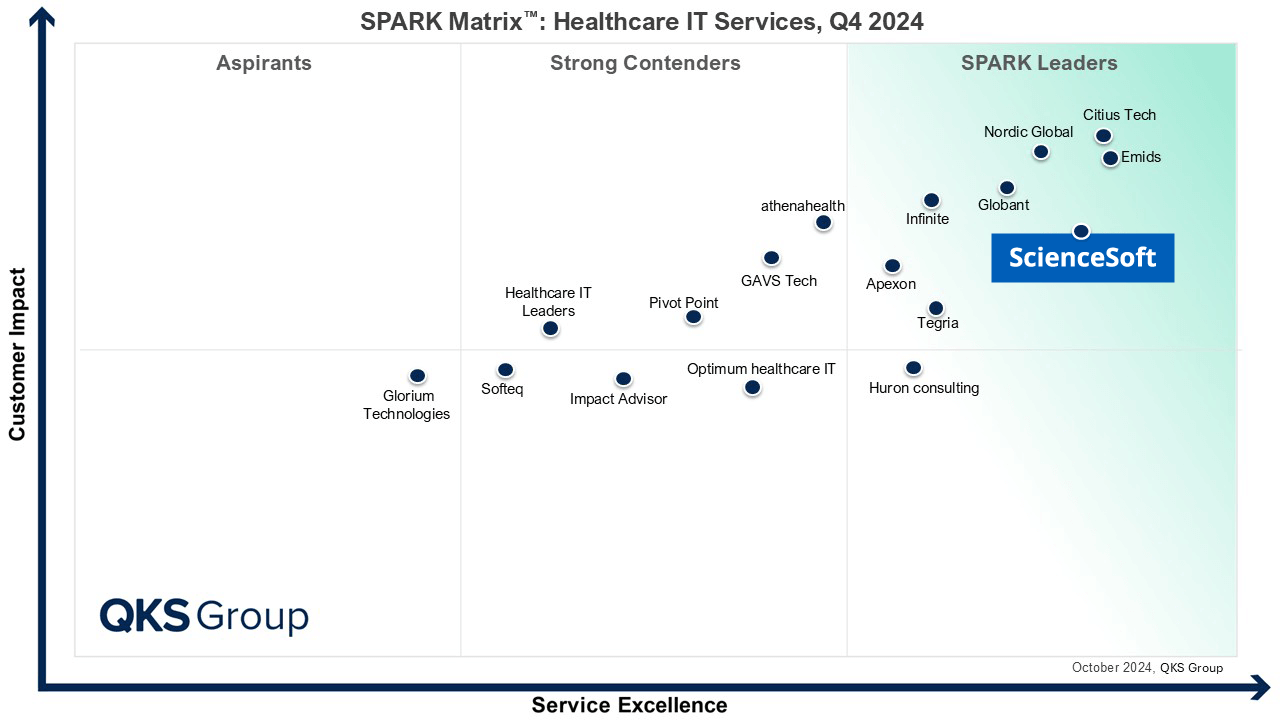
Featured among Healthcare IT Services Leaders in the 2022 and 2024 SPARK Matrix
Recognized for Healthcare Technology Leadership by Frost & Sullivan in 2023 and 2025
Named among America’s Fastest-Growing Companies by Financial Times, 5 years in a row

Top Healthcare IT Developer and Advisor by Black Book™ survey 2023
Four-time finalist across HTN Awards programs

Named to The Healthcare Technology Report’s Top 25 Healthcare Software Companies of 2025

HIMSS Gold member advancing digital healthcare
ISO 13485-certified quality management system
ISO 27001-certified security management system
About ScienceSoft
ScienceSoft is a US-headquartered international IT consulting and software development company founded in 1989. With 20 years of experience in healthcare IT and ISO 13485 certified quality management system, ScienceSoft is ready to deliver reliable telemedicine solutions for efficient care delivery in rural areas.