Insurance Fraud Detection Automation
Use Cases, Features, Costs, ROI
ScienceSoft brings 14 years of experience in insurance software engineering and digital transformation to help insurance firms establish robust automation of their fraud detection processes.
Insurance Fraud Detection Automation: Key Aspects
Insurance fraud detection automation helps streamline insurance data validation processes and promptly spot customer fraud and malicious employee activities. Insurance fraud detection systems can be powered by artificial intelligence (AI) to enable precise, analytics-based recognition and proactive prevention of suspicious transactions, identity theft, document forgery, and non-compliant workflows.
- Implementation time: 9–15+ months for a custom fraud detection automation system.
- Necessary integrations: customer interaction channels, claim management software, underwriting software, a policy administration system, accounting software.
- Development costs: $200K–$800K+, depending on software complexity. Use our cost calculator to estimate the cost for your case.
- Average payback period: <7 months.
- ROI: 200%–1,000%.
How to Automate Fraud Detection Across 8 Major Risk Areas
Identity fraud detection
Get automated customer identity verification to eliminate manual routines across client data processing, ensure compliance with KYC/AML regulations, and prevent unauthorized access to insurance services.
Underwriting fraud detection
Monitor the way your underwriters estimate risks and approve insurance applications. Be notified immediately if underwriting does not comply with internal and legal guidelines.
Policy data fraud detection
Establish intelligent validation of policy data to make sure there are no non-existent beneficiaries, the value of the insured assets is not inflated, and the risk information is accurate and complete.
Policy manipulation fraud detection
Get instant alerts on the attempts to create, change, or share insurance policies by unauthorized parties to block bad actors fast and prevent document fraud and sensitive data leakage.
Claim fraud detection
Leverage AI-powered validation of claim data and automated detection of fraudulent cases to get faster and more accurate claim decisioning, cut investigation efforts, and prevent undue and inflated payouts.
Sourcing fraud detection
Obtain full visibility of your damage handling partner selection activities and automatically identify suspicious agreements and payment transactions that failed to pass the pre-set approval flow.
Reinsurance fraud detection
Monitor reinsurance transactions and agent behavior to quickly spot an unusually large number of reinsurance agreements or policy replacements that can signal potential fee churning.
Accounting fraud detection
Employ automation to instantly detect and prevent malicious manipulations across business-critical financial data and ensure consistent and compliant financial reporting.
Common Insurance Fraud Schemes Software Helps Recognize
Customer identity theft
Document forgery
Misrepresenting risk data
Car insurance fronting
Premium diversion
Inventing losses
Claim misclassification
Claim exaggeration
Double billing
Fee churning
Key Features of an Automated Insurance Fraud Detection System
ScienceSoft designs and builds fraud detection solutions with functionality bound to each company’s specific needs. Below, our consultants outline the features commonly requested by our clients from the insurance industry:

See How Agentic AI Powers Insurance Fraud Detection
Watch how ScienceSoft’s custom AI agent applies voice intelligence and sentiment analysis to uncover fraud during conversational claim verification. Built on AWS Bedrock AgentCore and powered by OpenAI’s leading LLMs, the agent boosts investigator capacity by over 40% and drives 20%+ higher fraud detection rates through nuanced discrepancy indicators.
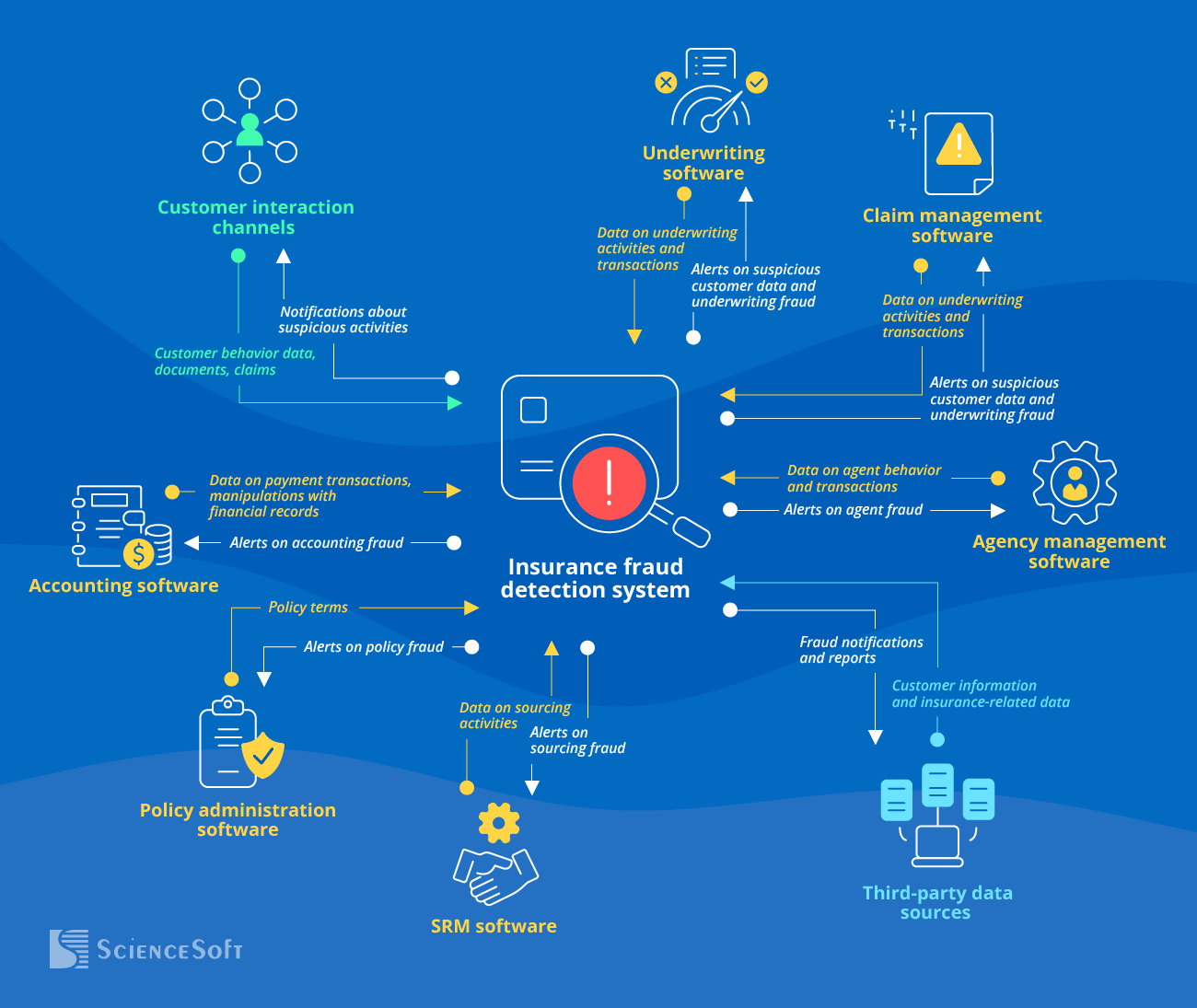
Essential Integrations for an Automated Insurance Fraud Detection System
Integrating insurance fraud detection software with the relevant systems helps eliminate manual aggregation and processing of insurance data and accelerate the identification of fraud cases. ScienceSoft recommends setting up the following integrations:
Customer interaction channels
To instantly spot suspicious customer behavior, faked documents and claims.
Show more
Corporate systems
What is not possible with configuration, we achieve with custom coding.
Show more
Third-party data sources
For data-driven validation of the information submitted by customers.
Show more
How to Drive High Payback From Insurance Fraud Detection Automation
Below, ScienceSoft’s consultants list the important factors that help unlock 1,000%+ ROI for automated insurance fraud detection.
AI-powered fraud analytics
Traditional ML and modern GenAI algorithms help recognize known and emerging insurance fraud schemes, including AI-produced identity deepfakes and forged documents. AI models continuously learn from new data to improve fraud detection accuracy.
ROI drivers: 20-40%+ improvement in fraud detection accuracy.
Maximized degree of automation
End-to-end automation of evidence gathering, validation, pattern checks across various types of fraud, and insight summarizing frees investigators from tedious manual routines and reduces case review timelines, letting insurers surface fraud faster.
ROI drivers: 5x lift in investigator capacity, up to 50x faster fraud spotting.
Accurate formalization of compliance rules
Converting internal and legal compliance requirements into clear automation rules gives software a consistent basis for detecting non-compliant servicing workflows and illegitimate customer transactions.
Integration with multiple data sources
Connecting fraud detection software to corporate systems and third-party data sources, including non-standard ones like IoT devices and social media, helps quickly obtain comprehensive data on customer and employee behaviors.

Agentic AI as the next big value driver
Watch the presentation by ScienceSoft’s Head of AI, Vadim Belski, from the 2025 Insurance Transformation Summit in Boston to explore how agentic AI can improve insurance claims fraud detection and what insurers need to deploy AI agents smoothly and safely.
How Much It Costs to Establish Insurance Fraud Detection Automation
Implementing insurance fraud detection automation for a midsize company may cost around $200,000–$800,000+, depending on the scope and complexity of the automation solution and the number of integrations.
Below, we provide the approximate cost estimations based on ScienceSoft's experience in fraud detection software projects:
$200,000–$400,000
Building a custom insurance fraud detection solution of average complexity that:
- Spots customer fraud across 1–3 insurance areas: onboarding, payments, claims, etc.
- Integrates with 1–5 corporate and external systems.
- Enables batch and real-time data processing.
- Enables diagnostic and predictive insurance analytics using statistical and non-neural-network ML models.
$400,000–$800,000+
Developing a comprehensive custom insurance fraud detection system that:
- Monitors fraud and non-compliance across multiple insurance areas.
- Integrates with 5+ back-office and third-party systems.
- Features real-time big data analytics for instant fraud detection.
- Provides root cause analysis and forecasting using deep learning models.
- Offers prescriptive fraud handling.
Key Financial Outcomes of Insurance Fraud Detection Automation
When to Opt for Custom Insurance Fraud Detection Software
ScienceSoft’s experts recommend building a custom insurance fraud detection automation system in the following cases:
- You need to automate complex or unique fraud detection workflows, for example:
- Verifying insurance workflow compliance with internal policies and local regulations.
- Capturing and analyzing claim-relevant data in various formats, including voice recordings, handwritten text, video, IoT device readings.
- Validating loss estimates for specific insurance types, such as professional liability insurance or natural disaster insurance.
- You want to employ value-adding technologies, such as agentic AI or smart contracts for automated insurance fraud detection.
- You want smooth and cost-effective integration of your insurance fraud solution with all the required software, including legacy insurance tools and third-party systems.
- You need a flexible solution that can be easily evolved with new capabilities to support sustainable business growth and quickly adapt to regulatory compliance changes.
Insurance Fraud Detection Automation Services by ScienceSoft
Why Automate Insurance Fraud Detection With ScienceSoft
-
Since 2012 in engineering custom software solutions for the insurance industry.
- Insurance IT and compliance consultants (NAIC, NYDFS, CCPA, GDPR, etc.) with 5–20 years of experience.
- 45+ certified project managers (PMP, PSM I, PSPO I, ICP-APM) who succeeded in large-scale projects for Fortune 500 firms.
- Principal architects with hands-on experience in designing complex insurance automation systems and driving secure implementation of value-adding technologies.
- 350+ software engineers, 50% of whom are seniors or leads.
- Established practices to ensure the high quality of insurance solutions and their delivery on the agreed timelines and budget, despite project constraints or uncertain requirements.
About ScienceSoft
ScienceSoft is a global IT consulting and software development company headquartered in McKinney, Texas. In insurance IT since 2012, we help insurance companies implement effective fraud detection automation. Being an ISO 9001- and ISO 27001-certified vendor, we apply a mature quality management system and guarantee that cooperation with us does not pose any risks to our clients’ data security.





